Nephrogenic systemic fibrosis and its association with gadolinium exposure during MRI
ABSTRACTNephrogenic systemic fibrosis (NSF) is a newly recognized systemic disorder characterized by widespread tissue fibrosis in patients with impaired renal function. Recent reports suggest that NSF is associated with exposure to gadolinium-based contrast agents used in magnetic resonance imaging. NSF can be very debilitating and can lead to serious complications and death. Health care providers should exercise caution when considering the use of gadolinium-based imaging studies in patients with renal dysfunction.
KEY POINTS
- NSF seems to arise in roughly 3% of patients with renal insufficiency who receive gadolinium, although the data are somewhat sketchy and the true incidence might be higher if the NSF is specifically looked for.
- Manufacturers of all available gadolinium contrast agents now must include a boxed warning about the risk of NSF in patients with acute or chronic severe renal insufficiency (glomerular filtration rate < 30 mL/minute/1.73 m2) and in patients with acute renal insufficiency of any severity due to hepatorenal syndrome or in the perioperative liver transplantation period.
- As yet, we have no effective treatment for NSF. If the patient is already on hemodialysis, it may be reasonable to perform hemodialysis immediately after exposure to gadolinium and again the next day.
A cross-sectional study
As mentioned above, Todd et al8 examined 186 dialysis patients for cutaneous changes of NSF (using a scoring system based on hyper-pigmentation, hardening, and tethering of skin on the extremities). Patients who had been exposed to gadolinium had a higher risk of developing these skin changes than did nonexposed patients (odds ratio 14.7, 95% confidence interval 1.9–117.0). More importantly, the investigators found cutaneous changes of NSF in 25 (13%) of the 186 patients, 4 of whom had prior skin biopsies available for review, each revealing the histologic changes of NSF. This study suggests that NSF may be more prevalent than previously thought.
Is kidney dysfunction always present?
All the reported patients with NSF had underlying renal impairment. The renal dysfunction ranged from acute kidney injury to advanced chronic kidney disease (estimated GFR < 30 mL/minute/1.73 m2) and end-stage renal disease on renal replacement therapy, ie, hemodialysis or peritoneal dialysis. The incidence of NSF does not seem to be related to the cause of the underlying kidney disease.
What other diseases or comorbidities can be associated with NSF?
It is still unclear why not every patient with advanced renal failure develops NSF after exposure to gadolinium.
A variety of complex diseases and conditions have been reported to be associated with NSF, with no clear-cut evidence of causality or trigger. These include hypercoagulability states, thrombotic events, surgical procedures (especially those with reconstructive vascular components), calciphylaxis, kidney transplantation, hepatic disease (hepatorenal syndrome, liver transplantation, and hepatitis B and C), idiopathic pulmonary fibrosis, systemic lupus erythematosus, hypothyroidism, elevated serum ionized calcium or serum phosphate, hyperparathyroidism, and metabolic acidosis. A possible explanation is that most of these conditions are associated with an increased use of MRI or MRA testing (eg, in the workup for kidney or liver transplantation).
Many drugs have also been reported to be associated with NSF, including high-dose erythropoietin,20 sevelamer (Renagel),21 and, conversely, lack of angiotensin-converting enzyme inhibitor therapy,22 but none of these findings has been reproduced to date.
GADOLINIUM CHARACTERISTICS AND PHARMACOKINETICS
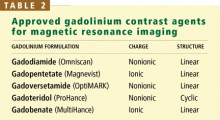
Gadolinium is a rare-earth lanthanide metallic element (atomic number 64) that is used in MRI and MRA because of its paramagnetic properties that enhance the quality of imaging. Its ionic form (Gd3+) is highly toxic if injected intravenously, so it is typically bound to a “chelate” to decrease its toxicity.23 The chelate stabilizes Gd3+ and thereby prevents its dissociation in vivo. These Gd-chelates can be classified (Table 2) according to their charge (ionic vs nonionic) and their structure (linear vs cyclic).
Most of the reported cases of NSF have been in patients who received gadodiamide, a nonionic, linear agent. Why gadodiamide has the highest rates of association with NSF is still unclear; perhaps it is simply the most widely used agent. Also, linear Gd compounds may be less stable and more likely to dissociate in vivo. The updated FDA Public Health Advisory in May 2007 warned against the use of all gadolinium-containing contrast agents for MRI, not just gadodiamide.
After intravenous injection, Gd-chelate equilibrates rapidly (within 2 hours) in the extracellular space. Very little of it enters into cells or binds to proteins. It is eliminated unchanged in the glomerular filtrate with no tubular secretion. In a study by Joffe et al,24 the elimination half-life of gadodiamide in patients with severely reduced renal function was considerably longer than in healthy volunteers (34.3 hours ± 22.9 vs 1.3 hours ± 0.25).
Since gadolinium compounds are not protein-bound and have a limited volume of distribution, they are typically removed by hemodialysis. Joffe et al found that an average of 65% of the gadodiamide was removed in a single hemodialysis session. However, they did not describe the specific features of the hemodialysis session, and it took four hemodialysis treatments to remove 99% of a single dose of gadolinium.24 A dialysis membrane with high permeability (large pores) seems to increase the clearance of the Gd-chelate during hemodialysis.25
Peritoneal dialysis may not remove gadolinium as effectively: Joffe et al24 reported that after 22 days of continuous ambulatory peritoneal dialysis, only 69% of the total amount of gadodiamide had been excreted, suggesting a very low peritoneal clearance.
SPECULATIVE PATHOGENESIS
Although a causal relationship between gadolinium use in patients with renal dysfunction and NSF has not been definitively established, the data derived from case reports assuredly raise this suspicion. Furthermore, on biopsy, gadolinium can be found in the skin of patients with NSF, adding evidence of causality.26–28
The mechanism by which Gd3+ might trigger NSF is still not understood. A plausible speculation is that if renal function is reduced, the half-life of the Gd-chelate molecule is significantly increased, as is the chance of Gd3+ dissociating from its chelate, leading to increased tissue exposure. Vascular trauma and endothelial dysfunction may allow free Gd3+ to enter tissues more easily, where macrophages phagocytose the metal, produce local profibrotic cytokines, and send out signals that recruit circulating fibrocytes to the tissues. Once in tissues, circulating fibrocytes induce a fibrosing process that is indistinguishable from normal scar formation.29