Update on constipation: One treatment does not fit all
ABSTRACTConstipation is a common clinical problem that can be difficult to manage. It has a variety of identifiable causes, but even idiopathic constipation has different possible mechanisms. Often, the key to improvement and patient satisfaction is to understand the mechanism and the patient.
KEY POINTS
- A high-fiber diet often improves functional constipation, but it may worsen slow-transit constipation or dyssynergia (a failure of the pelvic floor muscles to relax). Nevertheless, fiber remains a mainstay of treatment for its ability to provide homogeneous stool consistency.
- Drugs approved for treating constipation increase fluid in the lumen, speed intestinal transit, and improve stool consistency, while tegaserod (Zelnorm) additionally acts as a serotonin agonist.
- Colonoscopy and other tests are reserved for patients with refractory constipation and those with symptoms suggesting colon cancer.
- Prebiotics (short-chain carbohydrates that stimulate activity of beneficial colonic bacterial flora) and probiotics (live bacterial preparations) are under evaluation as treatments for chronic constipation.
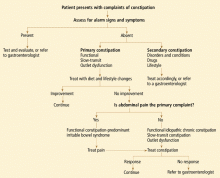
STRATEGIES FOR MANAGING CHRONIC CONSTIPATION
In the absence of secondary causes, treatment of chronic constipation is focused on relieving symptoms.
If symptoms are refractory to these traditional treatments, agents such as lactulose and polyethylene glycol may provide relief.11,21 Although they do not address the underlying cause of constipation, these agents increase the fluid content of the intestine, contributing to improved stool consistency, and consequently increase the frequency of bowel movements.
Lubiprostone similarly increases the fluid content of the colon, contributing to improved stool consistency, reduced fecal transit time, and increased frequency of bowel movements.66,70,102 Unlike lactulose and polyethylene glycol, which are indicated only for short-term use, lubiprostone has been found to be safe and effective when used for up to 48 weeks.70,71
Biofeedback is the preferred treatment for pelvic floor dyssynergia, in which it has a success rate of 70% to 81% and in which it is superior to standard treatment (laxatives, fiber, and education).103–105 In an instrument-based training program, patients receive auditory or visual feedback or both to help train the pelvic floor and relax the anal sphincter while simulating defecation. It also improves rectal sensation to assist in proper evacuation. The best outcomes are achieved when committed patients receive instruction from empathetic, properly trained physical therapists or other technicians. Studies show that the benefits of biofeedback are long-lasting.104 It does not improve slow-transit constipation, though pelvic floor dyssynergia and slow-transit constipation can overlap.