Evolution and results of aortic valve surgery, and a ‘disruptive’ technology
Disruptive technologies are innovations that are quickly adopted and that change long-established practices. One example is coronary stenting; another that is emerging is percutaneous aortic valve insertion. The latter is already benefiting patients who would not be able to undergo open heart surgery for valve replacement. However, the technology is still so new that we do not yet know how to define who will benefit from it.
VALVE SURGERY CONTINUES TO IMPROVE
Yet despite these excellent results, 30% to 61% of patients with severe symptomatic aortic valve stenosis do not undergo surgical aortic valve replacement because age and comorbid diseases put them at unacceptably high risk, or because they do not want it, or because they were never referred for it.
This concern about high risk is certainly justified, since age and comorbid conditions such as coronary artery disease, oxygen-dependent chronic pulmonary disease, renal disease, and peripheral vascular disease clearly have an adverse affect on outcome. For example, the risk of stroke and death is markedly higher in patients with peripheral vascular disease.1 It was because of the strong influence of comorbid disease in the elderly that we and others4,6 developed the novel approach of replacing the aortic valve with a stented valve via a catheter.
SURGICAL RISK IS HARD TO PREDICT
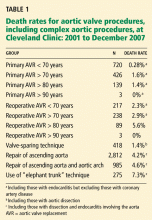
Decisions about which patients are at very high surgical risk or cannot undergo surgery are often somewhat subjective, based on a surgeon’s own experience.4,6 An algorithm for predicting operative outcomes, the Society for Thoracic Surgery equation score, is a reliable way to calculate the risk of death in patients in need of aortic valve replacement. Another method, the EuroScore, has been shown to be less predictive: in an audit of data for the multicenter Placement of Aortic Transcatheter Valves (PARTNER) trial currently under way to analyze results with these procedures, in 4,892 patients undergoing open surgical repair at Cleveland Clinic and considered at high risk (EuroScore > 10), the calculated expected risk of death was 26%, but the observed death rate was 10.9%—only 42% of the expected rate.
In my personal audit of the last 594 patients who underwent open surgical aortic valve replacement and were considered to be at high risk, the expected risk of death (as calculated by the EuroScore) was 27%, but the observed risk was considerably lower at 7%—only 26% of the predicted rate.