Percutaneous treatment of aortic valve stenosis
ABSTRACTAortic valve replacement via open heart surgery, although still the standard treatment for severe symptomatic aortic valve stenosis, is not an option for many patients with severe symptoms, and these patients are often left with suboptimal strategies such as medical management or balloon valvuloplasty. But over the last 5 years improvements in percutaneous approaches to implantation of prosthetic aortic valves have made it a potential therapeutic option for these patients. Technical and device issues are being refined, and percutaneous aortic valve replacement is showing promise in ongoing clinical trials.
KEY POINTS
- Aortic stenosis is the most common valvular condition, affecting 3% of the general population; its incidence and prevalence are increasing as the population ages.
- Many patients with severe aortic valve stenosis are considered too high-risk for standard surgical valve replacement but may be candidates for percutaneous valve replacement.
- Of the approaches now undergoing refinement, the most promising is retrograde (ie, femoral arterial) placement of the Edwards SAPIEN valve or the CoreValve.
- The technology is still evolving, and the learning curve is substantial, yet cautious enthusiasm about percutaneous aortic valve replacement is justified.
Stenosis of the aortic valve has a long, latent, asymptomatic phase, but when symptoms finally occur, clinical deterioration can be rapid. For patients with severe stenosis, the standard treatment has long been replacement of the aortic valve via open heart surgery. But many patients with severe stenosis are considered too high-risk for this procedure.
Until about 5 years ago, these patients had no other option but medical therapy or percutaneous aortic balloon valvuloplasty as a palliative measure or as a bridge to open heart surgery. But 5 years of experience with percutaneous techniques to implant prosthetic aortic valves show that this less-invasive approach may become a viable option for patients with severe symptomatic aortic valve stenosis.
In this review, we discuss current prosthetic valves and percutaneous techniques and their relative advantages and limitations and the potential future role of this new treatment option.
THE NEED FOR A LESS-INVASIVE APPROACH
Calcific aortic stenosis is the most common valvular heart disease, affecting 2% to 4% of adults over age 65 in the United States alone.1,2 The aging of our population and the lack of drug therapies to prevent, halt, or effectively slow aortic valve stenosis are leading to a greater burden of this condition.1,3,4 Already in the United States more than 50,000 surgical aortic valve replacements are performed every year for severe aortic stenosis.1,2 The associated in-hospital death rate is 8.8% in patients over age 65 years, and as high as 13% in low-volume centers.1,5
The steady increase in the number of patients requiring aortic valve replacement, the high surgical risk in patients with multiple comorbidities, the reluctance of some patients to undergo the trauma and pain associated with open heart surgery via sternotomy, and the fact that percutaneous procedures are less traumatic and offer faster recovery and fewer hospital days—all these are forces that have been driving the development of percutaneous techniques for the treatment of aortic stenosis.6–11 In addition, a recent study12 showed that 33% of patients over age 75 were deemed too high-risk for open heart surgery and thus were left untreated.12
The evolution of percutaneous aortic valve replacement
The idea of percutaneous treatment of aortic stenosis was first put into clinical practice in 1985, when Cribier performed an aortic balloon valvuloplasty.6 This was followed in 200013 by the first successful implantation of a catheter-based stent valve in a human, and in 2002 by the first successful percutaneous aortic valve replacement in a human.13–15 In the following sections, we discuss the percutaneous approaches in current use for the treatment of degenerative aortic stenosis.
AORTIC BALLOON VALVULOPLASTY
Percutaneous aortic balloon valvuloplasty, partial dilation of the stenotic aortic valve with a balloon inserted via a catheter,1,16–19 improves symptoms but has failed to show a sustained benefit on rates of mortality or morbidity.1,16–18 The restenosis rate is high, and symptoms recur in most patients within months to a year.1,16–18 Procedural complication rates are about 10%, and complication rates at the catheter access site are even higher.1,16–18 The 30-day death rate in the National Heart, Lung, and Blood Institute’s Balloon Valvuloplasty Registry, which included more than 600 patients, was 14%.18 In a retrospective study of 212 patients who underwent single or repeat percutaneous aortic balloon valvuloplasty,20 the 1-year mortality rate was 36% for the entire cohort, with a median survival of 3 years. Patients who underwent a repeat procedure (33%) had 1-year mortality rate of 42%, compared with 16% in patients who did not undergo a repeat procedure.20
Percutaneous aortic balloon valvuloplasty serves best as palliative therapy in severely symptomatic patients, and as a bridge to surgery in hemodynamically unstable adult patients.21,22 Percutaneous aortic balloon valvuloplasty is not an option in patients who are good candidates for surgical valve replacement.1
PERCUTANEOUS AORTIC VALVE REPLACEMENT: THREE TECHNIQUES
The antegrade technique
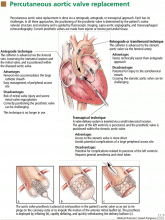
The retrograde technique
In the retrograde (ie, transfemoral) technique, access to the femoral artery is gained and the catheter with the prosthetic aortic valve is advanced to the stenotic aortic valve.8,11,26,28–30 This approach is faster and technically easier than the antegrade approach, but it can be associated with injury to the aortofemoral vessels and with failure of the prosthesis to cross the aortic arch or the stenotic aortic valve.11,23,30