A dermatologist’s skin tips for rheumatologists
EXPERT ANALYSIS FROM RWCS 2016
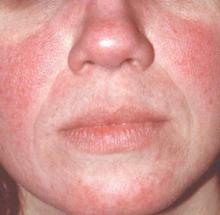
MAUI, HAWAII – Before concluding that a patient’s erythematous facial butterfly rash is an open and shut case of acute cutaneous lupus erythematosus, consider this, Dr. George M. Martin advised: 10-15 million Americans have acne rosacea.
“The 1% of those acne rosacea patients with the most severe disease are very often walking around misdiagnosed as having the butterfly rash of lupus,” Dr. Martin said at the 2016 Rheumatology Winter Clinical Symposium.
Indeed, rosacea – particularly the erythrotelangiectatic subtype – is the skin disease most often confused with acute cutaneous lupus erythematosus (ACLE), noted Dr. Martin, symposium codirector and a dermatologist practicing on Maui.
That’s a particularly common mistake in the event an individual with severe acne rosacea also happens to have the musculoskeletal symptoms of fibromyalgia, another very common disorder.
One clue useful in separating erythrotelangiectatic rosacea from ACLE is that “usually patients with the butterfly rash of acute lupus are sick. Rosacea patients are out there playing tennis and having a good time with a little bit of flush,” he said.
Other causes of a butterfly rash that get mistaken for ACLE are sebhorrheic dermatitis, contact dermatitis, and a photosensitizing drug eruption.
A biopsy may be necessary to establish a diagnosis, especially if the possibility of fibromyalgia is muddying the waters, according to Dr. Martin.
But cutaneous clues can also be helpful in deciding whether a butterfly rash is due to ACLE or cutaneous dermatomyositis. In lupus the rash typically spares the nasolabial folds, while the facial rash of dermatomyositis involves them. On the hands, the rash of ACLE spares the knuckles, whereas one-third of patients with dermatomyositis have the scaly red lesions known as Gottron’s papules over their knuckles. Cutaneous dermatomyositis has a predilection for the scalp, knees, and elbows.
A key distinction is that patients will report that the skin lesions of dermatomyositis are very itchy or have a burning sensation; that’s uncommon in cutaneous LE.
Also, prominent nailfold microhemorrhages at the distal cuticle are a telltale clue of dermatomyositis or possibly systemic sclerosis but aren’t part of the clinical picture in cutaneous LE. These microvascular changes are actually hemosiderin-containing deposits.
A skin biopsy is unhelpful in distinguishing cutaneous LE from cutaneous dermatomyositis. They basically have the same histopathologic findings, an interface dermatitis. Moreover, direct immunofluorescence and antinuclear antibody testing can be positive in both.
Dermatomyositis is more difficult to treat successfully than is cutaneous lupus. Antimalarials are often ineffective. But dapsone at 100-200 mg/day often works well in dermatomyositis, and it’s a relatively inexpensive drug, Dr. Martin said.
The hallmarks of subacute cutaneous lupus erythematosus (SCLE) are photosensitivity and small erythematous papules that expand into scaly patches and plaques that resemble psoriasis. SCLE is most common in women up to about age 40. It’s a disorder that predominates from the neck down. If more inflammation is present on the patient’s face than on the neck, shoulders, and upper torso, it’s not SCLE.
SCLE can be either drug induced or idiopathic; the two forms don’t differ clinically or histopathologically. In a patient older than age 50, SCLE is most commonly a drug-related eruption. In a 2011 review, Dr. Richard D. Sontheimer and his coinvestigators reported that antihypertensive agents accounted for one-third of cases of drug-induced SCLE, antifungals for one-quarter, chemotherapeutic agents for less than 9%, and antihistamines for 8% (Br J Dermatol. 2011 Mar;164[3]:465-72).
Dr. Sontheimer, professor of dermatology at the University of Utah in Salt Lake City, recently told Dr. Martin that his soon-to-be-published follow-up study of new cases since 2011 shows big changes in the culprit drugs. The proportion associated with chemotherapeutic agents, proton pump inhibitors, or biologics has jumped sharply. And with proton pump inhibitors now available over the counter, that class of medication is likely to continue to grow in importance as a source of drug-induced SCLE.
Dr. Martin reported serving on scientific advisory boards for and/or as a consultant to nine pharmaceutical companies.