Benzodiazepines for substance abusers
Do addiction worries outweigh the need for effective anxiety treatment? A sobriety-based algorithm addresses both concerns.
ILLICIT USE POTENTIAL
Prescriptions are the primary source of supply for benzodiazepine abusers. These patients are doctor shoppers and often change pharmacies. They visit emergency rooms frequently and may feign symptoms to obtain benzodiazepine prescriptions. They fill prescriptions for personal use or sell the drugs to illicit sources to support their addictions.
On the street, brand-name benzodiazepines are worth much more than generics because they can be identified by photographs of brand-name benzodiazepines on the Internet or in reference books. In many cities, the street value of the Xanax or Klonopin brands may be $5 to $10 per pill. A 5mg tablet of Valium-brand diazepam may sell for $5, and 10-mg tablets are worth up to $10.
Higher abuse potential. All benzodiazepines have abuse potential, and most have been reported in the literature as being abused. Those most likely to be abused have a short half-life10 (Table 1) or rapidly cross the blood brain barrier, such as alprazolam.11
Alprazolam and lorazepam are popular among benzodiazepine abusers. In experienced but nondependent users, 1 mg of alprazolam produces a sense of elation and carries an abuse potential similar to that of 10 mg of dextroamphetamine.12 Lipophilic agents such as diazepam also have a high abuse and addiction potential.
In the United States, diazepam and alprazolam appear to be the most abused benzodi-azepines.13 Flunitrazepam has become popular among high school students and drug addicts, particularly in the south and southwest. This potent benzodiazepine is not approved for use in the United States but is diverted from Latin America or Europe in the illegal drug trade.
Lower abuse potential. Benzodiazepines with longer half-lives generally are less likely to be abused, although diazepam—with a half-life of up to 100 hours—is the exception. Chlordiazepoxide has been reported to produce a lower “high” than other benzodiazepines.14 Among the short half-life benzodiazepines, oxazepam may have a relatively low abuse potential.14 Clonazepam—a high-potency benzodiazepine with a long half-life—is generally safe and may have a lower abuse or addiction potential, although its abuse has been report-ed.15 Similarly, oxazepam, clorazepate, and chlordiazepoxide may be less reinforcing than other benzodiazepines, although reports have linked these agents to abuse as well.16
TO PRESCRIBE OR NOT TO PRESCRIBE
Opponents blame benzodiazepines for promoting the drug culture and argue that prescribing benzodiazepines promotes drug abuse. Advocates of benzodiazepine therapy contend that restricting an effective and safe medication is unethical, even in substance abusers. Arguments from each perspective are summarized in Table 2.17-27
In 1990, an American Psychiatric Association task force concluded that alcohol and substance abusers could be prescribed benzodiazepines with very close monitoring but did not recommend specific standards.28
RECOMMENDATIONS
Prescribing benzodiazepines to substance abusers is not absolutely contraindicated, despite an elevated relative risk of abuse or dependence. In the absence of convincing data, physicians must decide on their own—usually case by case—the merits of using benzodiazepines to treat anxiety in substance abusers.
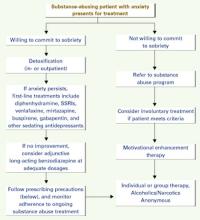
A sobriety-based approach. Our group at the Substance Abuse Treatment Center, VA Medical Center, Omaha, Nebraska, has developed a treatment algorithm for substance abusers presenting with anxiety (see Algorithm). It is based on clinical experience, more than 200 relevant articles, and the consensus of psychiatrists trained and certified by the American Board of Psychiatry and Neurology and the American Society of Addiction Medicine.
Algorithm Sobriety-based protocol for treating anxiety in substance abusers
Precautions for prescribing benzodiazepines
- Inform patient of planned duration of therapy
- Prescribe for brief periods (weeks to months), with follow-up at least monthly
- No refills without follow-up, and no refills over the phone
- Use random urine toxicology screening every 1 to 3 months to monitor for relapse
- Attempt to taper dosage after 3 to 6 months—even if patient resists—and monitor for objective withdrawal
- If no objective withdrawal, terminate benzodiazepine; continue other medications
- If objective withdrawal, continue benzodiazepine and reattempt taper in 3 to 6 months; continue Alcoholics/Narcotics Anonymous
We suggest that you begin by encouraging sobriety and referring willing patients to detoxification. Because most addicts deny or greatly minimize their substance abuse, investigate all potential drug or alcohol abuse thoroughly and address it appropriately.
If anxiety persists after detoxification, begin drug therapy with nonbenzodiazepines:
- Diphenhydramine, 50 to 100 mg/d, may reduce anxiety and often improves sleep, but consider its anticholinergic side effects before prescribing.
- Some SSRIs and venlafaxine are used to treat anxiety, but they generally take weeks to produce a therapeutic effect and some patients cannot wait that long.
- Mirtazapine, 15 to 30 mg/d, provides relatively rapid sedation and helps with sleep and anxiety.
- Buspirone may reduce anxiety, especially when given at 30 to 60 mg/d.
- Gabapentin, 100 to 300 mg tid or higher, may reduce anxiety and help with sleep.
- Tricyclic antidepressants may be considered, but watch for cardiac and anticholinergic side effects and overdose risks.