Interventions to Improve Follow-Up of Laboratory Test Results Pending at Discharge: A Systematic Review
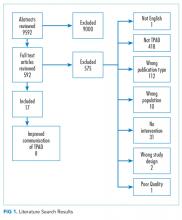
Failure to follow up test results pending at discharge (TPAD) from hospitals or emergency departments is a major patient safety concern. The purpose of this review is to systematically evaluate the effectiveness of interventions to improve follow-up of laboratory TPAD. We conducted literature searches in PubMed, CINAHL, Cochrane, and EMBASE using search terms for relevant health care settings, transition of patient care, laboratory tests, communication, and pending or missed tests. We solicited unpublished studies from the clinical laboratory community and excluded articles that did not address transitions between settings, did not include an intervention, or were not related to laboratory TPAD. We also excluded letters, editorials, commentaries, abstracts, case reports, and case series. Of the 9,592 abstracts retrieved, 8 met the inclusion criteria and reported the successful communication of TPAD. A team member abstracted predetermined data elements from each study, and a senior scientist reviewed the abstraction. Two experienced reviewers independently appraised the quality of each study using published LMBP™ A-6 scoring criteria. We assessed the body of evidence using the A-6 methodology, and the evidence suggested that electronic tools or one-on-one education increased documentation of pending tests in discharge summaries. We also found that automated notifications improved awareness of TPAD. The interventions were supported by suggestive evidence; this type of evidence is below the level of evidence required for LMBP™ recommendations. We encourage additional research into the impact of these interventions on key processes and health outcomes.
© 2018 Society of Hospital Medicine
Asking the Question
The full review, which is available from the corresponding author, assessed the evidence that the interventions improved (1) the timeliness of follow-up of TPAD or reduced adverse health events; (2) discharge planning, documentation, or communication with the outpatient care provider regarding TPAD; and (3) health outcomes. In this article, we present the impact of interventions to improve the documentation, communication, and follow-up of TPAD. The review protocol, which is also available from the corresponding author, was developed with the input of a panel of experts (Appendix A) in laboratory medicine, systematic reviews, informatics, and patient safety. The analytic framework (Appendix B) describes the scope of the review. The inclusion criteria for papers reporting on interventions to improve communication of TPAD are the following:
- Population: Patients who were admitted to an inpatient facility or who visited an ED (including patients released from the ED) and who had one or more TPADs.
- Interventions: Practices that explicitly aimed to improve the documentation, communication, or follow-up of TPAD, alone or as part of a broader quality improvement effort.
- Comparators: Standard practice, pre-intervention practice, or any other valid comparator.
- Outcomes: Documentation completeness, physician awareness of pending tests, or follow-up of TPAD.
Acquire the Evidence
A professional librarian conducted literature searches in PubMed, CINAHL, Cochrane, and EMBASE using terms that captured relevant health care settings, transition of patient care, laboratory tests, communication, and pending or missed tests (Appendix C). Citations were also identified by expert panel members and by manual searches of bibliographies of relevant studies. We included studies published in English in 2005 or later. We sought unpublished studies through expert panelists and queries to relevant professional organizations.
Appraise the Studies
Two independent reviewers evaluated each retrieved citation for inclusion. We excluded articles that (1) did not explicitly address laboratory TPAD; (2) were letters, editorials, commentaries, or abstracts; (3) did not address transition between settings; (4) did not include an intervention; (5) were case reports or case series; or (6) were not published in English. A team member abstracted predetermined data elements (Appendix D) from each included study, and a senior scientist reviewed the abstraction. Two senior scientists independently scored the quality of the eligible studies on the A-6 domains of study characteristics, practice description, outcome measures, and results and findings; studies scored below 4 points on a 10-point scale were excluded. Based on this appraisal, studies were classified as good, fair, or poor; poor studies were excluded.
Analyze the Evidence
We synthesized the evidence by intervention type and outcome. The strength of the evidence that each intervention improved the desired outcome was rated in accordance with the A-6 methodology as high, moderate, suggestive, or insufficient based on the number of studies, the study ratings, and the consistency and magnitude of the effect size.