Shared Decision-Making During Inpatient Rounds: Opportunities for Improvement in Patient Engagement and Communication
BACKGROUND: Shared decision-making (SDM) improves patient engagement and may improve outpatient health outcomes. Little is known about inpatient SDM.
OBJECTIVE: To assess overall quality, provider behaviors, and contextual predictors of SDM during inpatient rounds on medicine and pediatrics hospitalist services.
DESIGN: A 12-week, cross-sectional, single-blinded observational study of team SDM behaviors during rounds, followed by semistructured patient interviews.
SETTING: Two large quaternary care academic medical centers.
PARTICIPANTS: Thirty-five inpatient teams (18 medicine, 17 pediatrics) and 254 unique patient encounters (117 medicine, 137 pediatrics).
INTERVENTION: Observational study.
MEASUREMENTS: We used a 9-item Rochester Participatory Decision-Making Scale (RPAD) measured team-level SDM behaviors. Same-day interviews using a modified RPAD assessed patient perceptions of SDM.
RESULTS: Characteristics associated with increased SDM in the multivariate analysis included the following: service, patient gender, timing of rounds during patient’s hospital stay, and amount of time rounding per patient (P < .05). The most frequently observed behaviors across all services included explaining the clinical issue and matching medical language to the patient’s level of understanding. The least frequently observed behaviors included checking understanding of the patient’s point of view, examining barriers to follow-through, and asking if the patient has any questions. Patients and guardians had substantially higher ratings for SDM quality compared to peer observers (7.2 vs 4.4 out of 9).
CONCLUSIONS: Important opportunities exist to improve inpatient SDM. Team size, number of learners, patient census, and type of decision being made did not affect SDM, suggesting that even large, busy services can perform SDM if properly trained.
© 2018 Society of Hospital Medicine
RESULTS
All Patient Encounters
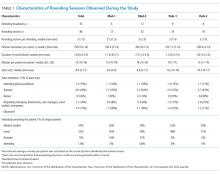
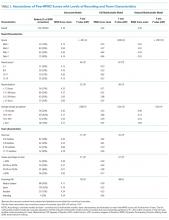
The median duration of rounding sessions was 1.8 hours, median patient census was 9, and median patient encounter was 13 minutes. The duration of rounds and minutes per patient were longest at Med-2 and shortest at Peds-1. See Table 1 for other team characteristics.
Peer Evaluations of SDM Encounters
Characteristics of Patients
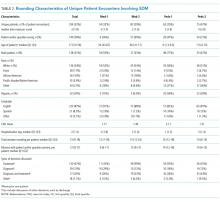
Teams spent a median of 13 minutes per SDM encounter, which was not higher than the round median. SDM topics discussed included 47% treatment, 15% diagnostic, 30% both treatment and diagnostic, and 7% other.
Variation in SDM Quality Among Attending Physicians
Overall Peer-RPAD Scores were normally distributed. After adjusting for the nested study design, the overall mean (standard error) score was 4.16 (0.11). Score variability among attendings differed significantly by service (LRT P = .0067). For example, raw scores were lower and more variable among attending physicians at Med-2 than other among attendings in other services (see Appendix Figure in Supporting Information). However, when service was included in the model as a fixed effect, mean scores varied significantly, from 3.0 at Med-2 to 4.7 at Med-1 (P < .0001), but the random variation among attendings no longer differed significantly by service (P = .13). This finding supports the hypothesis that service-level influences are stronger than influences of individual attending physicians, that is, that variation between services exceeded variation among attendings within service.
Aspects of SDM That Are More Prevalent on Rounds
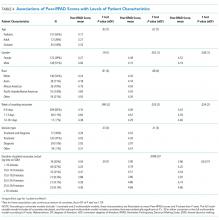
Rounds and Patient Characteristics Associated With Peer-RPAD Scores
Patient-RPAD Results: Dissimilar Perspectives of Patients and/or Guardians and Physician Observers
Among responders, mean Patient-RPAD scores were 6.8 to 7.1 for medicine services and 7.6 to 7.8 for pediatric services (P = .01). The overall mean Patient-RPAD score, 7.46, was significantly greater than the paired Peer-RPAD score by 3.5 (P = .011); however, correlations were not statistically significantly different from 0 (by service, each P > .12).
To understand drivers of the differences between Peer-RPAD and Patient-RPAD scores, we analyzed findings by item. Each mean patient-item score exceeded its peer counterpart (P ≤ .01; panel B of Figure). Peer-item scores fell below 33% on 2 items (Items 9 and 4) and only exceeded 67% on 2 items (Items 1 and 6), whereas patient-item scores ranged from 60% (Item 8) to 97% (Item 7). Three paired differences exceeded 50% (Items 9, 4, and 7) and 3 were below 20% (Items 6, 8 and 1), underlying the lack of correlation between peer and patient scores.