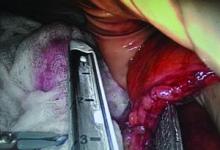
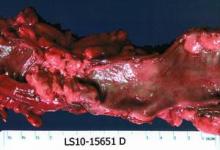
Bowel Resection With Invasive Endometriosis
Deep endometriosis involving the bowel is uncommon, but not rare, among patients with pelvic endometriosis. There is a growing body of literature describing minimally invasive colorectal resection for invasive endometriosis, and a growing feeling among gynecologic surgeons that endometriosis involving the rectal wall is better treated with rectal resection than with a shaving, or scraping, technique.
In our experience, by working within a multispecialty surgical team, that addressing endometriosis in a systematic fashion has led to a higher rate of patient satisfaction and quality of life, a lower rate of recurrent symptoms, and less surgical morbidity than has been seen with other approaches. While still infrequent, the greatest impact of this multispecialty approach has been the more liberal inclusion of bowel resection as part of the treatment for deep pelvic endometriosis.
It is our belief that patients who have evidence of bowel involvement and have a colorectal resection as part of their endometriosis treatment ultimately have a better surgical outcome. The opposite also appears to hold true. Those patients who have endometriosis involving the bowel wall and who do not receive a bowel resection have been more prone to recurrent disease and symptoms resulting in subsequent reoperations that are often more difficult to perform than a planned colorectal resection would have been.
Furthermore, surgery involving premeditated bowel resection is often safer than treatment employing a scraping technique when endometriosis is deep seated. In cases in which endometriosis has infiltrated the rectal wall, scraping techniques often result in unidentified bowel perforation, which leads to operations that are much more difficult to perform than planned elective resections. In addition, delayed missed injuries often will result in multiple trips to the operating room that frequently include the use of a colostomy in an otherwise young, healthy female patient.
Diagnosing Rectal Involvement
The full extent of disease, including the precise involvement of the bowel, sometimes can be difficult to determine prior to surgery. In many cases, however, physical examination combined with endoscopy and ultrasonography is enough to diagnose bowel involvement that would best be treated with segmental resection.
Pain associated with defecation, rectal bleeding around menses, and constipation often is found on history. On physical exam, endometriosis involving the rectal wall is most commonly associated with pain on both vaginal and rectal examination. Nodularity of the rectal wall, as well as distortion of the rectal folds, often are palpated.
The presence of either nodularity or rectal wall distortion raises the likelihood that there is significant rectal wall involvement. Conversely, if there is minimal or no nodularity of the rectal wall, the likelihood of rectal involvement is low.
When physical examination is abnormal, we proceed with colonoscopy, which enables us to visualize external compression on the rectal wall, nodularity, or other signs of endometriosis infiltrating the bowel wall. Colonoscopy is preferred because endometriosis is often found in the cecum, which would be missed on flexible sigmoidoscopy. Rarely will endometriosis actually penetrate the bowel wall. Most of the time, wall distortion with what is often seen as a submucosal mass is the only positive finding. Biopsy of the abnormality is typically unsatisfying, with normal colonic mucosa being the most common finding on microscopy.
When there are positive endoscopic findings, we prefer endorectal ultrasonography (ERUS) over transvaginal ultrasound to further evaluate rectal wall involvement of endometriosis. Using a 10 megahertz, 3-D ultrasound, we are able to visualize if endometriosis is attached to the bowel wall and to what degree.
The most important finding is whether or not endometriosis is invading the muscularis propria by the presence or absence of a space between the lesion(s) and the muscularis propria. If a space is visualized, there is a fairly good chance that the endometriosis may be safely scraped off the rectum.
If we see, on the other hand, that the endometriosis is either invading or firmly attached to the rectal muscularis propria, we know that chances of successfully scraping the lesion(s) off the rectum will be very low. In that case, a segmental resection of the rectum can be scheduled in conjunction with the rest of the endometriosis removal. Previous endometriosis surgery, it must be noted, leads to scar tissue which will often distort ERUS images and make the exam less accurate.
Surgical Planning
When the preoperative work-up is confirmatory, a combined surgical approach is scheduled. When the work-up is negative and the patient is scheduled for removal of endometriosis from the nongastrointestinal organs, we remain on surgical standby because bowel involvement of endometriosis is occasionally discovered in symptomatic patients despite a negative work-up.