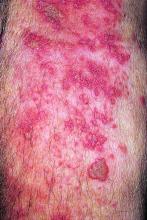
Cost equilibrium in Canada: Inpatient and outpatient treatment of herpes zoster
FROM BMC INFECTIOUS DISEASES
Rates of herpes zoster infections have increased substantially since the late 1990s in Canada. This, combined with rising per-episode medical costs and constant per-episode drug costs has led to increased total outpatient costs. But this has been offset by a dramatic drop in hospitalization rates and costs, according to a study published by BMC Infectious Diseases.
“A number of recent studies have looked at the burden of HZ-PHN [herpes zoster–postherpetic neuralgia] in a variety of health care systems, including Belgium, France, Germany, Greece, Italy, Spain, the United Kingdom, and Israel. However, little recent Canadian data have been published,” wrote Kevin J. Friesen, MD, and his associates at the University of Manitoba, Winnipeg, explaining that the goal of this study was to “establish the current burden of HZ and PHN in the setting of a universal health care system, and to look at long-term trends in their treatment costs.”
From 1997-1998 through 2013-2014, there were a total of 73,886 HZ incidents. In the final year alone, incidents numbered 5,746, which represents a 49.5% increase over 1997-1998. From the first year through 2009-2010, age-adjusted rates increased at a rate of 4.7 episodes per 1,000 person-years, but after that point, that rate increased to 5.7 episodes per 1,000 person-years, and continued that way through 2013-2014 (BMC Infect Dis. 2017. doi: 10.1186/s12879-017-2185-3).
Over the same 15-year time period, costs for drugs increased from an average of $89.77 to $127.34 per incident (P less than .03). Total medical costs increased from $57.98 to $78.84 per incident (P less than .00001).
However, the total annual cost of treating HZ and PHN dipped, particularly in 2011-2012, when it was $1,997,183, compared with $2,095,633 in the first year. Hospitalization rates also declined, going from 3.1% in 1997-1998 to 1.36% in 2011-2012 and bringing mean per-episode cost for the hospital down from $397 to $195.
“The combination of these trends in per-episode costs arising from medical care and drug treatment were multiplied by the increase in the annual incidence of HZ, causing total outpatient costs to increase,” the authors explained. “However, this increase was offset by the dramatic drop in rates of hospitalization and the resulting decrease in hospital costs.”
The study was funded by a grant from Merck Canada. Dr. Friesen and his coauthors did not report any relevant financial disclosures.