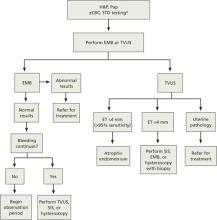
Postmenopausal bleeding: First steps in the workup
Is it endometrial cancer? When a postmenopausal woman presents with unexpected vaginal bleeding, this algorithm and review can help you answer that question without delay.
• Screen all women with postmenopausal vaginal bleeding (PMB) for endometrial cancer. A
• Use transvaginal ultrasound for the initial study for patients at low risk for endometrial cancer, and endometrial biopsy for those at higher risk. B
• Use saline infusion sonography as a second step in the evaluation of PMB if the diagnosis remains unclear after a biopsy or the bleeding persists despite a normal initial workup. B
Strength of recommendation (SOR)
A Good-quality patient-oriented evidence
B Inconsistent or limited-quality patient-oriented evidence
C Consensus, usual practice, opinion, disease-oriented evidence, case series
CASE Irene R, age 55, comes to see you because of vaginal bleeding, which started 7 days ago. The patient reports that she stopped menstruating about 4 years ago and is not on hormone replacement therapy or taking any medication. Irene, who is married and in a monogamous relationship with her husband of 20 years, denies any vaginal irritation, discharge, or dyspareunia. Her uterus is intact and she had a Pap smear about a year ago.
What will you include in a workup to determine the cause of her bleeding?
Endometrial cancer is the most common malignancy of the female reproductive organs, with more than 43,000 new cases detected in the United States in 2010 alone.1 More than half of all cases of endometrial cancer are diagnosed in women between the ages of 50 and 69 years.1,2
Vaginal bleeding, which more than 90% of women with endometrial cancer experience,3 is often the first sign of malignancy. Thus, all women who present with postmenopausal bleeding (PMB)—defined as any vaginal bleeding occurring ≥1 year after cessation of menses or any unscheduled bleeding in women on hormone replacement therapy (HRT)—require further evaluation.
Prognosis for endometrial cancer depends on the extent of the disease at the time of diagnosis. Most cases are diagnosed in the early stages and have a 5-year survival rate greater than 96%.1 Surgery alone can be curative if the malignancy is contained within the uterus.1,2
What are the essential elements of a workup for a woman with PMB? Which lab tests should be ordered and which procedures performed? You’ll find the answers in the at-a-glance ALGORITHM4-6 we created, and in the additional information provided in this evidence-based review.
ALGORITHM
Postmenopausal bleeding: An evidence-based workup4-6
CBC, complete blood count; EMB, endometrial biopsy; ET, endometrial thickness; H&P, history and physical; Pap, Papanicolaou smear; SIS, saline infusion sonography; STD, sexually transmitted disease; TVUS, transvaginal ultrasonography.
*Laboratory tests are generally not helpful in evaluating postmenopausal bleeding, but a complete blood count is warranted if bleeding is prolonged or heavy and a test for sexually transmitted diseases may be appropriate based on patient history or physical exam.
Endometrial cancer is the key concern
While endometrial cancer is the most serious cause of PMB, it is not the most common. Atrophic endometrium is the culprit 60% to 80% of the time, while endometrial cancer accounts for up to 10% of cases. Endometrial polyps or hyperplasia, HRT, and cervical cancer are among the conditions included in the differential diagnosis (TABLE).7
A workup for PMB starts with a thorough medical history and a physical examination, including a Pap smear to screen for cervical cancer. Results from the Pap smear may suggest other pathology, such as benign endometrial cells, atypical endometrial cells, or atypical glandular cells.
Is lab work necessary? Laboratory tests are generally not helpful in evaluating PMB itself. A complete blood count is warranted if the bleeding is prolonged or heavy, however, and testing for sexually transmitted diseases may be appropriate, based on the patient’s history and/or physical exam.5,8
TABLE
Postmenopausal bleeding: The differential diagnosis7
| Cause | Incidence (%) |
|---|---|
| Atrophic endometrium | 60-80 |
| HRT | 15-25 |
| Endometrial cancer | 7-10 |
| Endometrial hyperplasia | 5-10 |
| Polyp(s) (endometrial or cervical) | 2-12 |
| Miscellaneous (uterine leiomyomas, cervicitis, atrophic vaginitis, tamoxifen therapy, trauma, anticoagulation) | <10 |
| HRT, hormone replacement therapy. | |
Endometrial biopsy or transvaginal ultrasound: Which test is better?
For many years, dilatation and curettage (D&C) of the endometrium was standard practice in the evaluation of patients with PMB. The Society of Radiologists in Ultrasound (SRU) and the American College of Obstetricians and Gynecologists (ACOG) now advise starting with either endometrial biopsy (EMB) or transvaginal ultrasound (TVUS).4,6 Both procedures are more advantageous than D&C for evaluating PMB because they can be done in an outpatient setting, are less expensive, provide faster results, and correlate with surgical findings more than 95% of the time.9
Although numerous studies have attempted to define the roles of EMB with Pipelle and TVUS, the literature is unclear as to which initial test is preferable.
Endometrial biopsy. Many physicians prefer to start with EMB, because it provides tissue samples for a histological diagnosis, is easily performed, and causes minimal cramping. The test does have limitations, such as difficulty in obtaining adequate tissue samples.