Tools to speed your heel pain diagnosis
Quickly zero in on a diagnosis by using our handy “photo guide” and reference table.
- Advise patients with tendinopathy to decrease physical activity, do stretching exercises (C), undergo eccentric calf muscle training (B), use heel lifts (C), modify shoe fit, and take nonsteroidal anti-inflammatory drugs (NSAIDs) regularly for a few days, then as needed (B).
- The mainstay of treatment for calcaneal apophysitis in children is rest (C). Other options include heel lifts, stretching programs, icing, gel heel cups, and anti-inflammatory agents (C).
- Treatment options for plantar fasciitis include NSAIDs, stretching exercises, gel cups, arch supports, night splints, steroid injections, extracorporeal shock wave therapy, and surgery (B).
Strength of recommendation (SOR)
- Good-quality patient-oriented evidence
- Inconsistent or limited-quality patient-oriented evidence
- Consensus, usual practice, opinion, disease-oriented
One of your patients, a 40-year-old woman, recently began an exercise program, and she now says she has persistent heel pain. Your first suspicion is “another plantar fasciitis case.” However, after asking a few questions and performing a brief examination, you realize the problem is not what you expected. The pain is in the wrong place for plantar fasciitis and the patient’s history is atypical. How should you proceed?
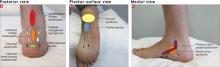
Knowing the precise location of maximum pain or tenderness (FIGURES 1A–1C) and pairing that with key findings from the exam and history (TABLE 1) can help you reach an accurate diagnosis and formulate proper treatment (TABLE 2).
Each of the 3 general areas of heel pain—posterior, plantar, and medial—introduces a unique differential. Bilateral symptoms or multiple joint involvement, of course, raises the possibility of associated systemic disease.
FIGURE 1
Common causes of heel pain by location
TABLE 1
A quick guide to narrowing your heel pain diagnosis
| AFFECTED AREA | ONSET OF PAIN | HISTORY AND KEY FINDINGS | LIKELY DIAGNOSIS |
|---|---|---|---|
| Posterior heel | Acute |
| Achilles rupture |
| Achilles strain | ||
| Chronic |
| Achilles tendinopathy | |
| Retrocalcaneal bursitis | ||
| Calcaneal apophysitis | ||
| Posterior impingement | ||
| Plantar surface | Acute |
| Calcaneal fracture |
| Plantar fascial rupture | ||
| Chronic |
| Plantar fasciitis | |
| Calcaneal stress fracture | ||
| Fat pad syndrome | ||
| Medial heel | Subacute |
| Posterior tibial tendonitis |
| Chronic |
| Posterior tibial tendon dysfunction | |
| Tarsal tunnel syndrome |
Posterior heel pain
The common causes of posterior heel pain are Achilles tendinopathy, retrocalcaneal bursitis, calcaneal apophysitis, posterior impingement (FIGURE 1A), and Achilles tendon strain or rupture. Rarer causes are sciatica, peroneal tendonitis, Haglund’s deformity, pump bump, and systemic disorders. The patient’s history and precise location of maximal tenderness1 differentiates these problems.
Achilles tendinopathy (tendonitis): Is the patient an athlete?
Insertional and noninsertional Achilles tendinopathy are the most common causes of persistent posterior heel pain.2,3 The inflammatory process occurs in the fatty tissue surrounding the Achilles tendon (the paratenon) rather than in the tendon itself. Patients tend to be highly active (often athletes) and may have recently increased their activity. Ask patients, too, whether they have recently taken a fluoroquinolone antibiotic. This drug class is known to increase the risk of both tendonitis and tendon rupture,4 and in July of this year the FDA directed drug manufacturers to add a black-box warning to that effect.5
Evaluation of noninsertional tendinopathy. Tenderness is usually located 2 to 6 cm above the Achilles insertion. Nodularity, swelling, or fluctuance of the tendon may be evident. Diagnosis generally can be made clinically. If confirmation is needed, consider ultrasonography or magnetic resonance imaging.
Treatment. Advise patients to decrease physical activity and do stretching exercises, undergo eccentric calf muscle training, use heel lifts, modify shoe fit, and use systemic or topical nonsteroidal anti-inflammatory drugs (NSAIDs) regularly for a few days, then as needed. Refractory cases may require surgery.6 New therapies that have proven effective include extracorporeal shock wave therapy (ESWT), prolotherapy (dextrose injections), and local application of nitroglycerin patches or gel.7-18 ESWT can be expensive and is not widely available. Prolotherapy can be performed with minimal training, but is still relatively new. Topical nitroglycerin is affordable, but beware of such side effects as headache and hypotension.
Evaluation of insertional tendinopathy. Inflammation occurs at the tendon’s insertion to bone (enthesitis). Pain typically is at the midline and is reproduced by palpating the tendon insertion or by passively stretching the heel. The presentation may be difficult to distinguish from retrocalcaneal bursitis (discussed below).
Treatment is similar to that used for noninsertional tendinopathy. However, if insertional tendinopathy occurs in conjunction with a Haglund’s deformity (bony overgrowth of the calcaneus), surgery may be indicated, because noninvasive measures tend to fail.19