Jet lag and shift work sleep disorders: How to help reset the internal clock
ABSTRACTJet lag sleep disorder and shift work sleep disorder are the result of dyssynchrony between the internal clock and the external light-dark cycle, brought on by rapid travel across time zones or by working a nonstandard schedule. Symptoms can be minimized by optimizing the sleep environment, by strategic avoidance of and exposure to light, and also with drug and behavioral therapies.
KEY POINTS
- Symptoms include daytime anergia, alternating complaints of insomnia and hypersomnia, emotional disturbances, and gastrointestinal distress. The severity depends on the degree and the duration of dyssynchrony, as well as on innate factors such as age and whether the patient is an “early bird” or a “night owl.”
- Drug treatment addresses sleep-related symptoms (eg, somnolence, insomnia) and attempts to hasten circadian reacclimation.
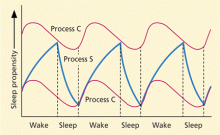
- Exposure to bright light in the hours leading up to the patient’s minimum core body temperature tends to push the internal clock later in time, whereas bright light in the hours immediately afterward pushes the clock earlier in time.
For people who must travel long distances east or west by air or who must work the night shift, some relief is possible for the grogginess and disorientation that often ensue. The problems arise from the body’s internal clock being out of sync with the sun. Part of the solution involves helping reset the internal clock, or sometimes, preventing it from resetting itself.
This review will focus on jet lag sleep disorder and shift work sleep disorder, with an emphasis on the causes, the clinical assessment, and evidence-based treatment options.
WHEN THE INTERNAL CLOCK IS OUT OF SYNC WITH THE SUN
Circadian rhythm sleep disorders are the result of dyssynchrony between the body’s internal clock and the external 24-hour light-dark cycle. Patients typically present with insomnia or excessive somnolence. These disorders may represent an intrinsic disorder, such as delayed or advanced sleep-phase disorder, or may be the result of transmeridian air travel or working nonstandard shifts.1
The intrinsic human circadian period is typically slightly longer than 24 hours,9 but it is synchronized (“entrained”) to the 24-hour day by various environmental inputs, or zeitgebers (German for “time-givers”), the most important of which is light exposure.10
When the internal clock is out of sync with the sun, the misalignment can result in daytime anergia, alternating complaints of insomnia and hypersomnia, and various other symptoms, including emotional disturbances and gastrointestinal distress. In particular, long-distance air travel or a nocturnal work schedule overwhelms the ability of the intrinsic clock to adjust rapidly enough, and the result is jet lag sleep disorder or shift work sleep disorder.1
TOOLS TO EVALUATE CIRCADIAN RHYTHM DISTURBANCES
A thorough history is the cornerstone of the evaluation for all sleep disorders, and if a circadian rhythm disturbance is suspected, the sleep history is supplemented with specific questions to establish a clear diagnosis.
When assessing for jet lag disorder, ask about:
- The patient’s degree of sleep deprivation before and during travel
- His or her innate circadian preference (ie, whether he or she is a “night owl” or “early bird”)
- Patterns of alcohol and caffeine consumption.
When assessing for shift work disorder, include the above questions and also look for differences in the sleep-wake schedule on working days vs nonworking days, as well as external contributors to poor sleep quality (eg, the degree to which daytime sleep is not “protected”).
The following tools help in acquiring this information.
Sleep diary
In a sleep diary or log, patients record the times that they take naps, maintain consolidated sleep, and subsequently arise. The diary also prompts the patient for information about sleep latency, wakefulness after sleep onset, time in bed, medication and caffeine intake, and the restorative quality of sleep.
While the sleep diary by itself may provide insight into counteractive sleep-related behaviors and misperceptions the patient may have, compliance is often limited. Therefore, the sleep diary is best used in conjunction with actigraphy.
Actigraphy
An actigraph is a wristwatch-size motion detector, typically worn continuously for 7 days or longer. The data it gathers and stores serve as a surrogate measure of various sleep-wake variables.11
Either a sleep diary or actigraphy is required to demonstrate the stability of sleep patterns and circadian preference, but the actigraph typically generates more reliable data.11,12 It is also valuable in assessing the response to treatment of circadian rhythm sleep disorders.13
Are you an early bird or a night owl?
The Morningness-Eveningness questionnaire contains 19 items. Night owls tend to score lower on it than early birds do.14 This information may help some people avoid situations in which they may not do well, such as an early bird going on a permanent night-shift schedule.
Other assessment tools
Polysomnography is used primarily to rule out sleep-disordered breathing; it is not indicated for routine evaluation of circadian rhythm sleep disorders.
The minimum core body temperature and the peak melatonin secretion follow a 24-hour cycle. Although these measures are often used in research, they are not routinely used in clinical practice. (The minimum core body temperature is discussed further below.)