Depression and heart failure: An overview of what we know and don’t know
ABSTRACT
Depression is prevalent in patients with heart failure, and the two conditions share underlying physiologic mechanisms. The prevalence of depression increases sharply with the severity of heart failure symptoms, an important consideration when confronting patients with worsening heart failure. Depression leads to poorer outcomes in patients with heart failure, including increased risk of poor functional status, hospital readmission, and death. Although beta-blockers are often implicated in the development and exacerbation of depression, evidence for this association is lacking, so withholding beta-blocker therapy is not recommended for patients with heart failure and depression. Evidence on whether therapy for depression also improves cardiac outcomes in heart failure patients is inconclusive, and further research on this question is needed. Nevertheless, early identification of depression in heart failure patients is imperative, as it can facilitate intervention attempts.
The relationship between depression and heart failure is not as obvious as the one between depression and coronary artery disease. Myriad questions on the subject are open to research:
- Does depression occur in heart failure at higher-than-expected rates?
- Does heart failure severity influence depression?
- Is depression a risk factor for heart failure? If so, why?
- How should we screen for depression in patients with heart failure?
- Do we have an evidence-based approach to treatment?
Part of the challenge in clarifying the relationship between depression and heart failure is that heart failure is a disease of chronically ill, elderly patients—a population in which adjustment disorder with depressed mood and major depression are also common diagnoses, with rates recently found to be 22.3% and 13.3%, respectively.1 Nevertheless, interest in examining the relationship between heart failure and depression is long-standing, and many clinical studies have examined this relationship.2–16 Unfortunately, measures are not standardized, so comparisons between studies are difficult.
DEPRESSION IS COMMON IN PATIENTS WITH HEART FAILURE
Many studies show that rates of depression among patients with heart failure are higher than expected among other elderly, chronically ill patients. Furthermore, depression has been linked to more severe heart failure symptoms and worse outcomes in some studies.
In a 2001 study, Jiang et al screened 374 hospitalized patients with heart failure using the Beck Depression Inventory score and found that 35% had scores of 10 or higher (indicative of at least mild depression).12 Further testing showed that 14% met criteria for major depression.
A 2006 meta-analysis of 27 studies by Rutledge et al found a 21% incidence of clinically significant depression in patients with heart failure.17 Rates of depression depended heavily on the rigor of screening criteria for classifying participants as depressed: rates were as high as 38% with the use of liberal criteria and as low as 14% with strict criteria. New York Heart Association (NYHA) functional status correlated strongly with the prevalence of depression, which increased steadily from 11% in patients with NYHA class I (mild) heart failure to 20% in those with class II, 38% in those with class III, and 42% in those with class IV (severe) heart failure.
In one of the studies included in the meta-analysis, Freedland et al found that the prevalence of major depression was strongly associated with age and functional status in hospitalized patients with heart failure.18 In patients younger than age 60 years, rates of major depression rose particularly sharply as heart failure symptoms worsened.
The Psychosocial Factors Outcome Study found that the prevalence of depression in patients with heart failure who participated in the community-based Sudden Cardiac Death in Heart Failure Trial (SCD-HeFT) was 36%, based on a score of 13 or greater on the Beck Depression Inventory-II.19 Similarly, unpublished preliminary data from the Heart Failure Adherence and Retention Trial (HART) show that about one-third of community-based patients with heart failure have depression.20
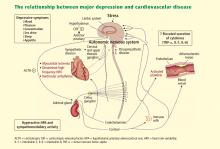
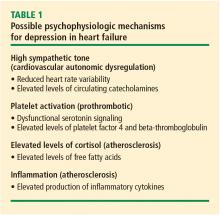
DEPRESSION AND HEART FAILURE ARE CLOSELY LINKED PHYSIOLOGICALLY
The evidence, therefore, strongly suggests a common pathway between heart failure and depression, and this evidence of a relationship favors a new paradigm that integrates the treatment of the two conditions.
BETA-BLOCKERS DO NOT RAISE RISK OF DEPRESSION
Pharmacotherapy is often implicated as a related factor in the development or exacerbation of depression in patients with heart failure, especially in those taking beta-blockers. Meta-analyses of the incidence of depression associated with various beta-blockers have been conducted in patients with hypertension, heart failure, and recent myocardial infarction. A 2002 meta-analysis of eight trials that randomized patients to treatment with a beta-blocker or placebo found no difference in the incidence of depressive symptoms between the active treatment and placebo groups, or between patients in the two groups who withdrew from the trial, presumably because of depression or other symptoms.24 An additional study not included in that meta-analysis found no differences in rates of depression among hypertensive patients according to the type of antihypertensive medication they were taking (ie, beta-blockers, diuretics, reserpine, or no drug therapy).25
Based on the evidence, I see no reason to avoid a trial of beta-blockers in patients who have depression at baseline or to be overly concerned that patients without depression will develop it as a result of beta-blocker treatment.