Menstrual manipulation: Options for suppressing the cycle
ABSTRACTMenstrual manipulation, ie, adjusting the menstrual cycle by taking hormonal contraceptives, allows women to have their period less often or to avoid bleeding at inconvenient times. The authors review the various options, the benefits, and the disadvantages of this practice.
KEY POINTS
- The options for menstrual manipulation are extended or continuous regimens of oral, transdermal, or vaginal hormonal contraceptives; a levonorgestrel-releasing intrauterine device; a progestin implant; and depot medroxyprogesterone injections.
- Benefits include fewer menstrual-related syndromes, less absenteeism from work or school, and greater overall satisfaction. Medical indications for it are conditions exacerbated by hormonal changes around the time of menses.
- The main disadvantage is a higher rate of breakthrough bleeding.
- Myths and misperceptions about menstrual manipulation persist; some physicians believe it is somehow inadvisable.
If they wish, women can have more control over when and if they menstruate. By using hormonal contraceptives in extended or continuous regimens, they can have their period less often, a practice called menstrual manipulation or menstrual suppression.
Actually, with the help of their clinicians, women have been doing this for years. But now that several products have been approved by the US Food and Drug Administration (FDA) specifically for use in extended or continuous regimens, the practice has become more widely accepted.
Reasons for suppressing menstrual flow range from avoiding bleeding during a particular event (eg, a wedding, graduation, or sports competition) to finding relief from dysmenorrhea or reducing or eliminating menstruation in the treatment of endometriosis, migraine, and other medical conditions exacerbated by hormonal changes around the time of menses.1 Alternatively, some women may practice menstrual manipulation for no other reason than to simply avoid menstruation.
MENSTRUAL DISORDERS ARE TROUBLESOME, COMMON
Each year in the United States, menstrual disorders such as dysmenorrhea (painful menstruation), menorrhagia (excessive or frequent menstruation), metrorrhagia (irregular menstruation), menometrorrhagia (excessive and irregular menstruation), and premenstrual syndrome affect nearly 2.5 million women age 18 to 50 years.2 Menstrual disorders are the leading cause of gynecologic morbidity in the United States, outnumbering adnexal masses (the second most common cause) by a factor of three.2 In addition, these disorders extend into the workplace, costing US industry about 8% of its total wage bill.3
A BRIEF HISTORY OF CONTRACEPTIVE DEVELOPMENT
The idea of using progestins for birth control was first advanced in the 1950s by Dr. Gregory Pincus, who proposed a regimen of 21 days of active drug followed by 7 drug-free days to allow withdrawal bleeding, mimicking the natural cycle.4 This “21/7” regimen was designed to follow the lunar cycle in the hope it would be, in the words of Dr. John Rock, “a morally permissible variant of the rhythm method,”5 thereby making it acceptable to women, clinicians, and the Catholic Church.
In 1977, Loudon et al6 reported the results of a study in which women took active pills for 84 days instead of 21 days, which reduced the frequency of menstruation to every 3 months. Since then, extending the active pills beyond 21 days to avoid menses and other hormone-withdrawal symptoms has become popular in clinical practice, and many studies have investigated the extended or continuous use of oral and other forms of contraception to delay menses.7–18
CURRENT METHODS OF MENSTRUAL MANIPULATION
A variety of available products prevent conception by altering the menstrual cycle:
- Oral estrogen-progestin contraceptive pills
- A drug-releasing intrauterine device
- Depot medroxyprogesterone acetate injections
- A contraceptive vaginal ring
- An implantable etonogestrel contraceptive.
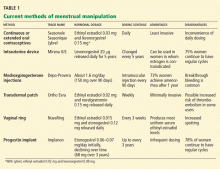
Their use in menstrual manipulation is summarized in Table 1.
Oral contraceptive pills
The most common way to manipulate the menstrual cycle is to extend the time between hormone-free weeks in an oral contraceptive regimen.
If the patient is young, you can prescribe a monophasic 21/7 oral contraceptive and tell her to take one active pill every day for 21 days and then start a new pack and keep taking active pills for up to 84 consecutive days, skipping the placebo pills until she wants to have her menstrual period. She can choose which week to have it: if the scheduled 12th week of an extended-cycle oral contraceptive regimen is inconvenient, she can plan it for week 10, or week 9, or whichever week is convenient.
The rationale for using an 84-day (12-week) cycle is that it still provides four periods per year, alleviating fears of hypertrophic endometrium.19
In this scenario, unscheduled or breakthrough bleeding can be managed by taking a “double-up pill” from a spare pack on any day breakthrough bleeding occurs and until it resolves. Menstrual periods should not be planned for intervals shorter than 21 days, owing to the risk of ovulation. Missed days of pills or use of placebo pills should also not exceed 7 days to prevent escape ovulation. 20
In some women with endometriosis and other medical reasons, continuous oral contraception with no placebo week can be prescribed.
Unfortunately, the downside to suppressing withdrawal bleeding is unscheduled or “breakthrough” bleeding. The best way to treat this unscheduled bleeding is not known. Patients who are not sexually active can be reassured that the goal of an atrophic endometrium can still be achieved, with resultant pill amenorrhea (particularly useful for those with severe dysmenorrhea or other reasons to want to avoid flow). Patients could also try to manage flow by periodically taking a 3- to 5-day break from hormone-containing pills to allow flow. They can also try switching to another oral contraceptive that has a different progestin that would spiral the arterioles of the endometrium more tightly and thus more aggressively induce atrophy.13,17,21 For instance, levonorgestrel is 10 to 20 times more potent than norethindrone. Choosing a pill with a higher monophasic dosing of levonorgestrel or a similar progestin may minimize unscheduled bleeding.
Currently, several oral contraceptives are approved for use in an extended regimen.
Seasonale was the first oral contraceptive marketed in the United States with an extended active regimen.22 It comes in a pack of 84 pills containing ethinyl estradiol 0.03 mg and levonorgestrel 0.15 mg, plus 7 placebo pills.
Seasonique is similar to Seasonale, but instead of placebo pills it has seven pills that contain ethinyl estradiol 0.010 mg.
Lybrel is a low-dose combination containing ethinyl estradiol 0.02 mg and levonorgestrel 0.09 mg. Packaged as an entire year’s worth of active pills to be taken continuously for 365 days without a placebo phase or pillfree interval,23 it is the only FDA-approved continuous oral contraceptive available in the United States.