Treating silent reflux disease does not improve poorly controlled asthma
ABSTRACTMany patients with asthma also have gastroesophageal reflux disease (GERD), and GERD can cause symptoms that mimic those of poorly controlled asthma. Patients with poorly controlled asthma are often treated empirically for GERD, whether or not they have symptomatic reflux. However, a randomized, placebo-controlled trial funded by the American Lung Association and the National Institutes of Health found that treating silent GERD does not improve asthma control. These results warrant a reevaluation of current guidelines and clinical practice.
KEY POINTS
- Acid reflux is more prevalent in patients with asthma, and it often occurs without classic symptoms such as heartburn.
- Current guidelines, based on data from older studies with significant limitations, recommend considering treatment for reflux disease, even without the classic symptoms, in patients with uncontrolled asthma.
- The recent Study of Acid Reflux in Asthma found not only that treating silent acid reflux does not improve asthma control, but also that esophageal pH monitoring does not detect a subgroup of asthma patients who might respond to a proton pump inhibitor. These data suggest that we should reconsider clinical practice based on current guidelines.
Should patients with poorly controlled asthma be treated empirically for gastroesphageal reflux disease (GERD)?
Current guidelines1 indicate that trying a proton pump inhibitor may be worthwhile. However, the results of a recent multicenter trial2 indicate that this does not help control asthma symptoms and that we need to reevaluate the guidelines and focus on other factors that can worsen asthma control.
REFLUX DISEASE IS LINKED TO ASTHMA
GERD’s association with asthma has long been recognized. Asthma patients have a higher prevalence of GERD than the general population, with reported rates of 20% to 80%.3–8
GERD may worsen asthma via several mechanisms. If stomach acid gets into the airway, it can induce bronchoconstriction, vagal reflexes, and chronic airway inflammation, all of which can increase airway reactivity.9–16 Chronic reflux can also cause inflammation of the esophagus, which can exacerbate cough and possibly bronchospasm via neurogenic mechanisms.17
In turn, asthma may worsen GERD. Airway restriction can lead to hyperinflation and increased negative inspiratory pleural pressure, both of which may reduce the effectiveness of the lower esophageal sphincter.18 In addition, the beta-agonists and methylxanthines used to treat asthma may impair function of the lower esophageal sphincter and exacerbate reflux.18–20
CURRENT GUIDELINES ARE BASED ON LIMITED INFORMATION
The symptoms of GERD and asthma are nonspecific and can be similar (chest tightness, chest discomfort), which can make it challenging for clinicians or patients to distinguish asthma from GERD.2 Moreover, in asthma patients, GERD often presents without classic symptoms such as heartburn, and thus has been labeled “silent” GERD.
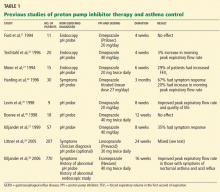
However, these studies all had significant limitations, such as small sample size. Also, the definitions of asthma and GERD differed from study to study. In some cases, the definition of GERD included self-reported GERD, which often fails to correlate with GERD documented with esophageal pH monitoring in asthma patients.1 These limitations were highlighted in a Cochrane review,30 which found that asthma patients with GERD showed no overall improvement in asthma after treatment of reflux. It concluded that small groups of patients may benefit, but that predicting who will respond is difficult.
Larger randomized controlled trials28,29 attempted to address some of these limitations, with varying results.
Littner et al29 gave lansoprazole (Prevacid) 30 mg twice daily or placebo to 207 patients with moderate to severe asthma and symptomatic GERD and saw no improvement in daily asthma symptoms, ie, asthma control in the active-treatment group. While these patients had an improvement in symptoms of severe reflux, their overall quality-of-life scores were similar to those of the placebo group. Of note, patients needing more than one type of drug for asthma control had a lower rate of asthma exacerbations.
Kiljander et al28 gave esomeprazole (Nexium) 40 mg twice daily or placebo to 770 patients who had mild to moderate asthma and symptoms of nocturnal asthma with or without symptoms of GERD. The only benefit was a slight improvement in peak expiratory flow in those with symptoms of both GERD and nocturnal asthma, and this was most significant in patients taking long-acting beta-agonists. Other measures—eg, the forced expiratory volume in the first second (FEV1), use of a beta-agonist, symptom scores, and nocturnal awakenings—did not improve.
In both of these studies,28,29 patients reported symptoms of GERD, so they did not have silent GERD.
THE DESIGN OF SARA
In SARA, 412 patients age 18 and older with inadequately controlled asthma were randomized to receive esomeprazole 40 mg twice a day or placebo for 24 weeks. Inadequate control was defined as a score of 1.5 or higher on the Juniper Asthma Control Questionnaire31 despite treatment with inhaled corticosteroids. Patients had no symptoms of GERD. The 40-mg twice-daily dosage of esomeprazole was chosen because it is known to suppress more than 90% of acid reflux.24,32
All patients completed a baseline asthma diary, recording peak expiratory flow rates, asthma symptoms, nighttime symptoms, and beta-agonist use. This information was collected every 4 weeks throughout the trial.
All participants also underwent esophageal pH monitoring for an objective confirmation of GERD. Patients were randomized independently of the results of the pH probe; in fact, investigators and patients were blinded to these results.
The primary outcome measure was the rate of episodes of poor asthma control, with poor control defined as any of the following:
- A decrease of 30% or more in the morning peak expiratory flow rate on 2 consecutive days, compared with the patient’s best rate during the run-in period
- An urgent visit, defined as an unscheduled health care visit, for asthma symptoms
- The need for a course of oral prednisone for treatment of asthma.
Asthma was defined as doctor-diagnosed, plus either a positive methacholine challenge test (a concentration of methacholine causing a 20% reduction in FEV1 [PC20] < 16 mg/mL) or a positive bronchodilator response (a 12% increase in FEV1) to an inhaled beta-agonist. Participants had no other indication for acid suppression, including symptoms of GERD or previously diagnosed erosive esophageal or gastric disease.
Acid reflux was evaluated by ambulatory pH monitoring, which had to last at least 16 hours and span one meal and 2 hours in the recumbent position. Reflux was present if the pH was less than 4.0 for more than 5.8% of total time, 8.2% of time upright, or 3.5% of time lying down.33 Episodes and severity were measured by the Gastroesophageal Reflux Disease Symptom Assessment Scale.34