Measles: Not just a childhood rash
ABSTRACTIn recent years, the number of US measles cases has increased, and outbreaks in adults continue to be reported in communities with a high number of unvaccinated people. These trends underscore the need for high overall measles vaccination coverage, and for physicians to entertain the diagnosis of measles in adult patients with a febrile illness and rash.
KEY POINTS
- Measles is one of the most contagious infectious diseases, with a secondary attack rate of at least 90% in susceptible household contacts.
- Since 1993, most reported cases of measles have been directly or indirectly linked to international travel, and many have occurred in adults.
- Acute measles encephalitis, a neurologic complication of measles, is more common in adults than in children and is characterized by the resurgence of fever during the convalescent phase, along with headaches, seizures, and altered consciousness.
Although measles is generally considered a disease of children, it affects people of all ages. While the incidence of measles in the United States is significantly lower than in 1963, when an effective measles vaccine was first introduced, recent increases in the number of sporadic cases and community outbreaks in adults show that measles is still a significant health problem.
PATHOGENESIS OF MEASLES
Measles is a highly contagious viral infection, whose manifestations have been recognized since the 7th century. The measles virus is an RNA virus of the Paramyxoviridae family. It is very difficult to isolate from clinical specimens, requiring special cell lines for in vitro propagation.
After acquisition, the measles virus establishes localized infection of the respiratory epithelium and then spreads to the regional lymphatics. A primary viremia then occurs, in which the virus replicates at the site of inoculation and in the reticuloendothelial tissues. A secondary viremia follows, in which the virus infects and replicates in the skin, conjunctiva, respiratory tract, and other distant organs.
The measles rash is thought to be due to a hypersensitivity reaction.1 Cell-mediated responses are the main line of defense against measles, as evidenced by the fact that people with cell-mediated deficiencies develop severe measles infection.2 Immunity to wild-type measles is believed to be lifelong.3,4
MEASLES IS HIGHLY CONTAGIOUS
Measles is one of the most contagious infectious diseases, with a secondary attack rate of at least 90% in susceptible household contacts. 4 The fact that emergency departments and physicians’ offices have become sites of measles transmission in recent years underscores the transmissibility of the virus.5–7
Although the virus is very labile, it can remain infective in respiratory droplets from the air for many hours. Thus, measles virus spreads from person to person by direct contact with droplets from respiratory secretions of infected persons.
The period of maximal contagion is the late prodrome, ie, 2 to 4 days before the onset of the rash. People who are generally in good health are contagious through 4 days after the onset of the rash, whereas people with compromised immunity can continue to shed the virus for the entire duration of the illness.
Airborne transmission precautions are required for 4 days after the onset of the rash in hospitalized, non-immunocompromised patients with measles, and for the duration of the illness for immunocompromised patients.
In the absence of widespread measles vaccination, measles infection peaks in late winter and early spring.
EPIDEMIOLOGIC TRENDS: CAUSE FOR CONCERN
Since an effective vaccine became available in 1963, the annual incidence of measles cases in the United States has decreased by more than 99%. A significant resurgence from 1989 to 1991 affected mainly unvaccinated preschoolers and resulted in more than 55,000 cases and 130 deaths.8 This resurgence prompted widespread, intensive immunization efforts and the recommendation that a second dose of measles vaccine be given to school-aged children. This led to the effective elimination of endemic transmission of measles in the United States.9
Although 90% of these cases either were directly imported or were associated with importation from other countries,10 the reason for the large number of cases was clearly the greater transmission after importation of the virus into the United States. This transmission was the direct result of the fact that 91% of the cases occurred in unvaccinated people or people whose vaccination status was not known or was not documented. A high proportion— at least 61 (47%)—of the 131 measles cases in 2008 were in school-aged children whose parents chose not to have them vaccinated. Although no deaths were reported in these 131 patients, 15 required hospitalization.
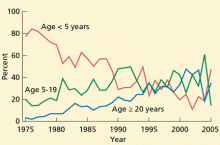
Although most reported measles cases are still in young and school-aged children, recent cases and outbreaks have also occurred in isolated communities of adults. Approximately 25% of the cases reported in 2008 were in people age 20 and older. Most adults who contracted measles had unknown or undocumented vaccination status. Similarly, a small measles outbreak occurred in Indiana in 2005, when an adolescent US citizen traveling in Europe became infected in Romania and exposed 500 people at a church gathering upon her return. Thirty-four cases of measles were reported from this exposure, and many were in adults.11
The recent increase in the number of cases reported and the continued reports of outbreaks highlight the fact that measles outbreaks can occur in communities with a high number of unvaccinated people, and underscore the need for high overall measles vaccination coverage to limit the spread of this infection.12