Approach to a low TSH level: Patience is a virtue
ABSTRACTConfronted with a low serum level of thyrotropin (thyroid-stimulating hormone, TSH), physicians should not jump to the conclusion that it is due to a hyperthyroid state, as other conditions and some drugs can be associated with a TSH level that is slightly low (0.1–0.4 μIU/mL) or frankly suppressed (< 0.1 μIU/mL). This review discusses how to approach a low TSH, stressing the frequent need to reassess thyroid function before making a diagnosis, the underlying processes and the drugs that can be responsible, and the degree of TSH suppression and its role in the evaluation.
KEY POINTS
- A low TSH value should always be followed up by measuring the thyroid hormones, ie, thyroxine (T4) and triiodothyronine (T3).
- Serum levels of free thyroid hormones should be used when interpreting an abnormal TSH level, especially in the acute and inpatient settings.
- A low TSH level is not always the result of suppression by elevations in circulating thyroid hormones.
- A low TSH level in the setting of normal levels of free thyroid hormones should always be reassessed in 4 to 6 weeks before making a diagnosis.
- Overt hyperthyroidism is usually associated with a frankly suppressed TSH (< 0.1 μIU/mL).
Elevated human chorionic gonadotropin
The alpha subunit of human chorionic gonadotropin (hCG) is homologous to the alpha subunit of TSH. Thus, hCG in high concentrations has mild thyroid-stimulating activity.
The serum hCG concentration is highest in the first trimester of pregnancy and hCG’s thyroid-stimulating activity can suppress the serum TSH level, but in most cases the TSH level remains within the “normal range” of pregnancy.21,22 The hCG levels observed during the first trimester of pregnancy are usually associated with a low TSH and normal free thyroid hormone levels. In pregnant women who are not on T4 therapy for hypothyroidism, a persistently suppressed TSH (< 0.1 μIU/mL) after the first trimester or elevations of the free thyroid hormones at any point during pregnancy suggest that the suppressed TSH is secondary to autonomous thyroid function, as seen in Graves disease and toxic nodular goiters, warranting further investigation. Iodine radioisotope imaging studies are forbidden during pregnancy.
If the hCG concentration is markedly elevated and for a prolonged time, as in hyperemesis gravidarum and gestational trophoblastic disease (hydatidiform mole, a benign condition, and choriocarcinoma, a malignant condition), overt hyperthyroidism can develop, with elevated free T4 and free T3.21,23
LOW TSH, NORMAL FREE T4, LOW FREE T3
Euthyroid sick syndrome and/or medication effect. When the TSH level is low secondary to euthyroid sick syndrome or a drug, or both, the free T3 level is usually found to be also low, which may be solely related to a component of euthyroid sick syndrome or secondary to the drugs themselves, as drugs such as corticosteroids and amiodarone inhibit the conversion of T4 to T3.
LOW TSH, NORMAL FREE T4, HIGH FREE T3
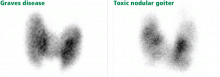
Toxic nodular goiter vs early Graves disease
If the free T3 is elevated and the TSH is low (suppressed), even in the absence of symptoms, a diagnosis of subclinical hyperthyroidism would be inappropriate, because by definition the free T4 and free T3 levels must be normal for a diagnosis of subclinical hyperthyroidism. The diagnostic possibilities are toxic nodular goiter and early Graves disease.
The combination of high T3, suppressed TSH, and normal T4 is usually associated with toxic nodular goiter, whereas T3 and T4 are typically both elevated in Graves disease (although T3 is usually more elevated than T4).24
The patient should also be tested for TSH receptor antibodies (TRAB), both stimulating and blocking, which are very specific for Graves disease.
Natural thyroid preparations
Natural thyroid preparations, which can contain large amounts of T3, can also yield the combination of normal free T4 and high free T3. Since these preparations contain both T4 and T3, they usually result in low TSH, normal free T4, and elevated free T3 levels when given in supratherapeutic doses. However, if these preparations are consumed in large enough quantities, both the free T4 and free T3 can be elevated. This is in contrast to supratherapeutic monotherapy with T3 (liothyronine), which usually results in low TSH, low free T4, and high free T3.