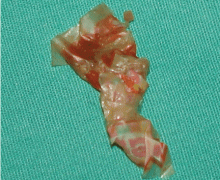
Pleural effusion from a candy wrapper
The patient is started on ceftriaxone (Rocephin) and levofloxacin (Levaquin). Left thoracentesis reveals blood-tinged exudative pleural fluid with 1.01 × 109/L nucleated cells, 43% neutrophils, 35% macrophages, and 15% lymphocytes; glucose and pH are normal. Pleural fluid culture is negative, and cytologic study does not reveal malignant cells. Computed tomography of the chest reveals consolidated pneumonia in the left upper lobe, with atelectasis of the left lower lobe and left pleural effusion. The combination of exudative pleural fluid with pH of 7.35, a glucose level of 87 mg/dL, a lactate dehydrogenase level of 406 U/L (normal range 100–200), negative microbiologic test results, and pneumonia supports the diagnosis of uncomplicated parapneumonic pleural effusion, which occurs in 40% of cases of bacterial pneumonia.
The patient could have been treated only for complicated left pneumonia with parapneumonic pleural effusion. But the high suspicion of foreign-body aspiration, with the history of mild mental retardation and previous recurrent right pneumonia, led to the further workup and appropriate treatment.
Risk factors for tracheobronchial foreign-body aspiration in adults are a depressed mental status or an impairment in the swallowing reflex.2
,Aspiration commonly occurs into the right lung because of the almost straight axis between the trachea and the right mainstem bronchus.3 However, aspiration can occur into any part of the lung depending on the position of the patient. Common foreign bodies described in adults are teeth or dental appliances, pins, and semisolid food, especially in elderly people.4 The clinical presentation varies from dyspnea and wheezing to asphyxia and cardiac arrest. Unilateral wheezing—particularly in young children with asthma, cough, or cold symptoms—should raise suspicion of foreign body aspiration.
Delayed complications of bronchial obstruction manifest usually as pneumonia. Subsequently, pleural effusion may develop because of an increased capillary permeability secondary to endothelial injury,5 and may progress to empyema.
Fiberoptic bronchoscopy has become the cornerstone of the diagnostic evaluation in adults with suspected foreign-body aspiration. Treatment options include extraction of the foreign body via flexible bronchoscopy or rigid bronchoscopy. Rigid bronchoscopy has higher success rates but requires general anesthesia.6
A history of choking is not always obtained. Imaging studies do not localize the foreign body in all cases. Many other medical conditions mimic breathing abnormalities similar to those associated with tracheobronchial foreign body in adults. Only a high index of suspicion can ensure proper diagnosis and treatment.