Nephrolithiasis: Treatment, causes, and prevention
ABSTRACTFactors that promote stone formation include low daily urine volumes; saturation of the urine with calcium, oxalate, calcium phosphate, uric acid, or cystine; acidic urine; and bacterial infection. The author identifies the mechanisms of stone formation and outlines management aimed at preventing recurrences.
KEY POINTS
- During an acute stone event, medical management focuses on pain control. Hydration and certain drugs may help the stone to pass.
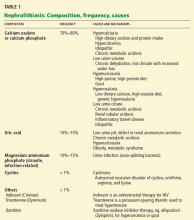
- Most stones are composed of calcium oxalate or calcium phosphate. Less common are uric acid, magnesium ammonium phosphate, and cystine stones.
- To prevent stones from recurring, patients who have had any type of stone should maintain an adequate fluid intake to keep the urine dilute.
- Paradoxically, calcium restriction is not warranted for patients who have had calcium stones, and may even be harmful.
- Alkalinization of the urine may help prevent recurrent uric acid stones and cystine stones.
COMMON AND ON THE INCREASE
Nephrolithiasis is common, with a lifetime prevalence of 10% in men and 5% in women.1,2 Studies have shown that the prevalence is increasing in the United States. In the second National Health and Nutrition Examination Survey (1988–1994), the prevalence in adults ages 20 to 74 was greater than in the 1976–1980 survey (5.2% vs 3.2%).3 The increase was observed in whites but not in African Americans or Mexican Americans, was greater in men than in women, and was greater with age in each time period.
In addition, stones often recur, and each stone event can be associated with significant metabolic and intervention-related morbidity.
PRESENTATION: SEVERE COLIC
Most patients present with moderate to severe colic, caused by the stone entering the ureter. Stones in the proximal (upper) ureter cause pain in the flank or anterior upper abdomen. When the stone reaches the distal third of the ureter, pain is noted in the ipsilateral testicle or labia. A stone at the junction of the ureter and the bladder often causes dysuria, urgency, and frequency and may be mistaken for a lower urinary tract infection.
Less often, patients present with silent ureteral obstruction, unexplained persistent urinary infection, or painless hematuria. However, even in patients with symptoms, the absence of hematuria does not exclude urolithiasis. In a study of 397 patients presenting with acute symptomatic urolithiasis, 9% did not have hematuria.4
The differential diagnosis in a patient with symptoms suggesting renal colic includes:
- Musculoskeletal pain
- Herpes zoster
- Diverticulitis
- Duodenal ulcer
- Cholecystitis
- Pyelonephritis
- Renal infarct
- Renal hemorrhage
- Gynecologic disorders
- Ureteral obstruction from renal papillary necrosis with sloughed papillae, a blood clot, or a ureteral stricture.
HELICAL CT WITHOUT CONTRAST IS THE PREFERED IMAGING STUDY
The diagnosis can be confirmed by computed tomography (CT), renal ultrasonography, or intravenous pyelography.
Helical CT without contrast is the preferred imaging study in patients with suspected nephrolithiasis. It has several advantages over other imaging studies: it requires no radiocontrast material; it shows the distal ureters; it can detect radiolucent stones (ie, uric acid stones), radio-opaque stones, and stones as small as 1 to 2 mm; and it can detect hydronephrosis and intra-abdominal and renal disorders other than stones that could be causing the patient’s symptoms.
In a study in 100 consecutive patients presenting to an emergency department with flank pain, helical CT had a sensitivity of 98%, a specificity of 100%, a positive predictive value of 100%, and a negative predictive value of 97% for the diagnosis of ureteral stones.5 In a study of 1,000 consecutive patients with suspected stones, helical CT identified significant, additional, or alternative reasons for the patient’s symptoms in 10% of cases.6
Ultrasonography has the advantage of not using radiation, but it is less sensitive for detecting stones and can image only the kidney and the proximal ureter. A retrospective study in 123 patients found that, compared with helical CT as the gold standard, ultrasonography had a sensitivity of 24% and a specificity of 90%.7 Ultrasonography may also miss stones smaller than 3 mm in diameter.
Conventional radiography (kidney-ureter-bladder view) is inadequate for diagnosis as it may miss stones in the kidney or ureter (even small radio-opaque stones) and provides no information about possible obstruction.
Intravenous pyelography has few advantages in renal lithiasis, exposes the patient to the risk of radiocontrast infusion and contrast-mediated acute renal injury, and gives less information than noncontrast CT.
MEDICAL MANAGEMENT OF ACUTE STONE EVENTS
Most stones are smaller than 5 mm and readily pass without interventions such as lithotripsy, ureteroscopy, or percutaneous nephrolithotomy. (For more information on these interventions, see the review by Samplaski and colleagues in this issue of the Cleveland Clinic Journal of Medicine.8)
Even if the stone is as large as 1 cm, I would let the patient try to pass it spontaneously if it is in the distal ureter, and I would allow up to 4 weeks for this to happen.
For most patients, pain management is paramount. Randomized controlled trials suggest that parenteral nonsteroidal anti-inflammatory drugs (NSAIDs) are as effective as narcotics for controlling the pain of renal colic.9 Diclofenac (Voltaren) has been used in several studies.
To hasten stone passage, some recommend inducing high urine flow with oral intake of at least 2 to 3 L of fluids per 24 hours to ensure a urine output of at least 2 L per day.
Drugs may also help the stone to pass. A recent study in 210 patients with ureteral stones averaging 6 mm in diameter showed that tamsulosin (Flomax) increased the likelihood of spontaneous stone passage.10 A meta-analysis of 693 patients in nine randomized trials concluded that alpha-blockers and calcium channel blockers increased the likelihood of stone passage compared with no treatment.11 Borghi et al,12 in a randomized, double-blind study in 86 patients with unilateral ureteral stones, reported a higher rate of stone passage in patients treated with methylprednisolone (Medrol) 16 mg/day plus nifedipine (Procardia) 40 mg/day than in those given methylprednisolone alone.