Hepatitis B: A strategy for evaluation and management
ABSTRACTIn hepatitis B virus (HBV) infection, a single approach to treatment cannot be applied to all patients. Acute, adult-acquired HBV infection rarely requires treatment, whereas treatment for chronic infection should be based on the patient’s clinical situation and test results. The ideal agent for treating hepatitis B does not exist, and trade-offs are the essence of agent selection. In last month’s Journal (Cleve Clin J Med 2008; 75:881–889), we outlined the natural history and diagnosis of chronic HBV infection; in this article we outline its management.
KEY POINTS
- Patients with HBV infection should be screened for hepatocellular carcinoma, especially if they have cirrhosis.
- Nucleoside and nucleotide analogue reverse transcriptase inhibitors are easy to use and therefore are usually the first-line therapy. Problems with these agents are that the optimal treatment duration is not known, and that drug resistance can emerge.
- Patients with advanced liver disease or hepatocellular carcinoma should be referred promptly for possible liver transplantation.
- Candidates for immunosuppressant therapy or cytotoxic chemotherapy should be screened for HBV, as this therapy can cause a potentially fatal flare of HBV.
- People at risk should be vaccinated; many have not been.
ANTIVIRAL THERAPY
Below, we summarize the main principles of anti-HBV therapy, emphasizing whether to treat and with which agent. Treatment of HBV infection in patients who are also infected with HIV or hepatitis C virus and in those with resistant or refractory hepatitis B is not within the scope of this article.
Acute infection rarely needs treatment
Acute, adult-acquired HBV infection is self-limited in most cases,1 and antiviral therapy is not routinely indicated.
In the rare cases of acute liver failure related to acute HBV infection, use of a nucleoside or nucleotide analogue reverse transcriptase inhibitor (nucleoside/nucleotide analogues) has been recommended, although no properly designed studies have been done.2,3 This recommendation is based on anecdotal experience, the relative safety of the antiviral agents, the serious nature of acute liver failure, and the possible need for emergency liver transplantation that requires prophylaxis against recurrence.
The nucleoside/nucleotide analogues that have been recommended in acute liver failure are lamivudine (Epivir), telbivudine (Tyzeka), and entecavir (Baraclude)—but not adefovir (Hepsera), which has a slow action and potential nephrotoxicity. Interferon drugs are contraindicated because they frequently cause side effects and can worsen hepatitis.4
Patients with acute liver failure should be referred promptly to a liver transplant center, and other management measures should also be started in a timely fashion.
In chronic HBV infection, treatment decisions are individualized
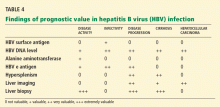
In chronic hepatitis B (ie, lasting > 6 months), treatment decisions should be based on the patient’s clinical situation and test results. The route and duration of infection (if known), history of previous hepatitis flares, ALT levels, current and previous HBV serologic test results and DNA levels, findings on liver biopsy (if previously done), and clinically suspected cirrhosis are all important to consider when deciding whether antiviral therapy is needed.
For many patients with chronic HBV infection, observation without antiviral therapy is warranted, eg:
- Young patients (< 30 years old) who acquired HBV at birth and who have persistently normal ALT levels with no evidence of advanced liver disease, regardless of their HBV DNA level (immune tolerance phase)
- Chronic inactive carriers who have no e antigen, persistently normal ALT levels, and very low or undetectable levels of HBV DNA without evidence of significant liver injury.
These patients can be managed by internists by close monitoring for hepatitis flares with serial ALT measurements along with other general management measures.
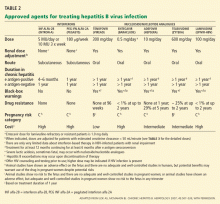
Antiviral agents for chronic HBV infection
An ideal agent for treating hepatitis B does not exist. Trade-offs are the essence of agent selection.
Interferons, the first drugs shown to be effective against HBV, can in some respects be considered the best available initial choice, especially in patients positive for hepatitis e antigen. Interferons have numerous side effects but, unlike all the other options, they have a well-defined duration of treatment (4–6 months in patients positive for e antigen). The principal goal of this therapy is disappearance of e antigen.
Interferon-based therapy is not recommended in patients with cirrhosis, however, because of the risk of hepatic decompensation associated with interferon-related flares of hepatitis.4
Although single-agent antiviral therapy may someday be replaced by a multidrug regimen, the data so far are not sufficiently robust to recommend multidrug regimens except possibly in cases of established drug resistance.
Adjunctive management
Vaccinations. All patients with chronic hepatitis B should be vaccinated against hepatitis A if serologic testing indicates they have no immunity to it. Influenza and pneumococcal vaccines are recommended for all patients with chronic liver disease.6
Alcohol rehabilitation. Patients who abuse alcohol should be counseled, and many need consultation with a psychosocial care provider for alcohol rehabilitation.
Smoking cessation. Cigarette smoking is linked to a higher risk of hepatocellular carcinoma in patients with chronic liver disease, including chronic HBV infection.7 Therefore, smokers should be counseled to quit.
Surveillance for hepatocellular carcinoma. Hepatocellular carcinoma can occur in patients with chronic hepatitis B, in most cases on top of cirrhosis, although important exceptions exist. The American Association for the Study of Liver Diseases recommends surveillance for hepatocellular carcinoma in all HBV carriers with cirrhosis and in the following groups regardless of whether they have cirrhosis8:
- Asian men age 40 and older
- Asian women age 50 and older
- African patients age 20 and older
- Patients with a family history of hepatocellular carcinoma
- Possibly, those with high HBV DNA levels and ongoing inflammatory activity.
In the United States, liver ultrasonography and alpha fetoprotein measurement every 6 to 12 months is a reasonable strategy.
If there is evidence of cirrhosis, esophagogastroduodenoscopy is recommended to screen for esophageal and gastric varices.