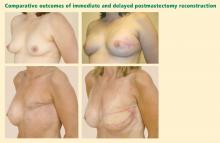
Options and considerations in the timing of breast reconstruction after mastectomy
ABSTRACT
Timing of breast reconstruction after mastectomy is determined primarily by patient factors and the need for postmastectomy radiation therapy. If the risk of needing postmastectomy radiation is low, then immediate reconstruction produces the optimal aesthetic result. If the risk of needing postmastectomy radiation is high, then delayed reconstruction is preferable to optimize both radiation delivery and aesthetic outcome. For patients with an increased risk of needing postmastectomy radiation, "delayed-immediate" reconstruction, which involves placing a tissue expander at the time of mastectomy and awaiting pathology results to determine the need for radiation and guide reconstruction scheduling, is a viable approach. Thorough and informed physician counseling about the pros and cons of these options is critical for all women undergoing mastectomy.
Accounting for adjuvant medical therapy
Preoperative evaluation and postoperative histologic lymph node status determine the potential need for adjuvant therapy and facilitate optimal surgical decision-making. Chemotherapy usually begins within 30 to 40 days after surgery but can be delayed up to 12 weeks. Thus, a reconstruction that will be healed within this time frame is ideal. Reconstruction choices that involve well-vascularized tissue will optimize healing prior to chemotherapy. Chemotherapy cannot be started in the presence of seroma, infection, or necrotic tissue. In cases of breast conservation surgery and radiation therapy only, radiation can be delayed up to 8 weeks for complete healing prior to its commencement.
In a patient who will require radiation, autologous reconstruction (using the patient’s own tissue) is preferable to tissue expander and implant reconstruction. Indications for radiation after mastectomy include tumor invasion of the chest wall, invasive cancers larger than 5 centimeters, and, in some cases, positive lymph nodes. Patients who undergo radiation of an autologous flap often have some shrinkage of the flap volume. Dense scar formation, capsular contraction, and implant extrusion may occur with radiation of implants, leading to a poor cosmetic outcome. Implant reconstructions that fail for these reasons are best corrected by autologous means.
Another consideration that should be addressed between the oncologic surgeon and the plastic surgeon is the possibility of an axillary lymph node dissection after reconstruction in the event of a positive sentinel node biopsy. If the oncologic surgeon must return to the axilla for removal of nodes after reconstruction, cooperation is needed between the two teams for incision planning and dissection. This is especially true in cases of microvascular free-tissue transfer reconstruction, in which vessels in the axilla are used for anastomosis. Recent data suggest that most microsurgery practitioners prefer to use the internal mammary vessels to avoid the need to return for another operation involving the axilla, which can jeopardize flap viability.6
DELAYED RECONSTRUCTION: A VIABLE OPTION REQUIRING REALISTIC EXPECTATIONS
Although reconstruction at the time of mastectomy is the preferred approach at present, delayed reconstruction in a patient who previously had a mastectomy is also a viable option. Since surgical therapy for breast cancer has been practiced long before reconstructive procedures were in widespread use, many patients were not offered any reconstructive options at the time of mastectomy. Other patients chose to delay reconstruction until after radiation therapy and/or chemotherapy were completed.
Why patients may choose to delay
Delayed reconstruction may be preferable for patients who are not ready to make a decision at the time of initial surgery as a result of the overwhelming news of their cancer diagnosis and the many treatment options they have to consider. These patients may benefit from first focusing on treatment of their cancer and reserving consideration of reconstruction for later. In other cases, patients with multiple medical comorbidities may benefit from a staged procedure to minimize the length of surgery. It should be recognized, however, that if reconstruction is not performed at the time of initial mastectomy, the likelihood that it ultimately will be performed may be significantly reduced.
What prompts the decision to eventually seek reconstruction?
The goals of patients seeking delayed reconstruction are numerous. Some express a desire to put the “cancer phase” of their life behind them, while others hope to escape the stigma of being different. Generally these women wish to think, feel, and carry on their lives as they did before their mastectomy. In addition, patients may desire a tangible, lasting result to symbolize that their treatment is finished. In the late phase of the recovery process, breast reconstruction may be viewed as a healthy route of return to the patient’s “normal” life before cancer.
It is important for mastectomy patients to know that they are still candidates for breast reconstruction as a delayed procedure, even if their mastectomy was performed in the distant past.