Overview of breast cancer staging and surgical treatment options
ABSTRACT
Following diagnosis of breast cancer, patients undergo assessment for local and systemic treatment. Establishing a relationship and communication with the patient is critical to this assessment, as are history-taking, clinical breast examination, review of imaging studies, and interactive discussion with the patient of treatment options and possible breast reconstruction. Some type of surgical therapy is indicated in virtually all women with breast cancer, generally as the first part of a multicomponent treatment plan. The main goal of surgical therapy is to remove the cancer and accurately define the stage of disease. Surgical options broadly consist of breast conservation therapy, generally followed by radiation therapy, or mastectomy. The surgical procedure also includes assessment of regional lymph nodes for metastasis, either by axillary lymph node dissection or by the less-invasive sentinel lymph node biopsy, for the purpose of cancer staging and guiding adjuvant therapy.
In the late 19th century, breast cancer was considered a fatal disease. That began to change in the 1880s when W.S. Halsted described the radical mastectomy as the way to treat patients with breast cancer.1 This aggressive surgical treatment—in which the breast, axillary lymph nodes, and chest muscles are all removed—remained the standard of care throughout much of the 20th century; as late as the early 1970s, nearly half (48%) of breast cancer patients were treated with radical mastectomy. During the 1970s, however, the Halsted radical mastectomy was largely abandoned for a less-disfiguring muscle-sparing technique called the modified radical mastectomy; by 1981, only 3% of patients underwent the Halsted mastectomy.2
The 1980s heralded even more minimally invasive techniques with the advent of breast conservation therapy, in which an incision is made over the tumor and the tumor is completely removed with negative margins, leaving behind normal breast tissue. (This procedure has been referred to by many different names, including definitive excision, lumpectomy, quadrantectomy, and partial mastectomy; since they all mean the same thing, for clarity and consistency this article will use “breast conservation therapy” throughout.) During the 1990s, surgical invasiveness was further minimized with the emergence of sentinel lymph node excision.
An important contributor to this evolution in the standard of breast cancer therapy since the 1970s has been the National Surgical Adjuvant Breast and Bowel Project (NSABP), a National Cancer Institute–funded clinical trials cooperative group. NSABP studies have been the driving force to show that the extent of surgery could be reduced without compromising outcome.3 These studies, along with several other trials, have resulted in a marked reduction in surgical aggressiveness and a multitude of adjuvant therapies for women with breast cancer. This article will briefly explore where this evolution has brought us in terms of the surgical options available for treatment of breast cancer today. We also discuss other key components in the management of women with newly diagnosed breast cancer, including cancer staging, patient counseling, and assessment of axillary lymph nodes.
BREAST CANCER CLASSIFICATION AND STAGING
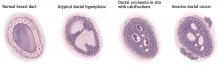
Pathologic classification
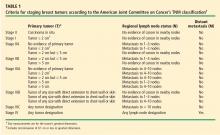
Cancer staging
A simpler method relies on the National Cancer Institute’s SEER (Surveillance, Epidemiology, and End Results) summary staging system.5 This system classifies tumors as “localized” (contained in the breast, either in situ or invasive), “regional” (identified in regional lymph nodes), or “metastatic” (spread to distant organ systems).
Of course, patients cannot be told their stage until after surgery, when a final pathologic report detailing tumor size and nodal status is available. Some patients will never be definitively staged—for instance, those who undergo neoadjuvant chemotherapy for locally advanced disease prior to lymph node dissection, or those who do not have a metastatic work-up. The metastatic work-up involves ordering of additional tests to assess for metastasis, but only when prompted by specific patient symptoms. Thus, if the patient has shortness of breath, a chest radiograph or a chest computed tomograph (CT) needs to be ordered; for elevated liver enzymes, CTs of the abdomen and pelvis are ordered; for central nervous system symptoms, brain magnetic resonance imaging (MRI) is ordered; and for back pain or bone pain, a bone scan is ordered to rule out metastatic disease to bone.
INITIAL PATIENT ASSESSMENT AND COUNSELING
Relationship-building is fundamental
Following an initial diagnosis of breast cancer, the patient must undergo an assessment for local and systemic disease. The surgeon, as a member of a multi-disciplinary breast cancer treatment team, often spearheads this initial assessment. This first visit must go beyond mere clinical evaluation, however, and include thorough discussion and relationship-building with the patient, as this early meeting establishes a relationship with the patient that will carry through her entire process of cancer care. For a true understanding between patient and surgeon to occur, it is critical for patients to be comfortable in sharing their fears, expectations, and lifestyle needs. Following a diagnosis of breast cancer, the initial reactions women go through include both fear and realization of one’s own mortality. Although these responses may no longer be justified by the reality of patient outcomes in most cases, they are normal and fully understandable reactions. For this reason, clinicians must be sensitive to these reactions while being supportive about the efficacy of the treatment options available.