The painful knee: Choosing the right imaging test
ABSTRACTThe initial evaluation of acute knee pain should include plain radiography, which is a quick and cost-effective way to identify a wide range of problems, including fracture, degenerative changes, osteochondral defects, and effusions. Computed tomography (CT) is the test of choice to better delineate fractures in patients who have knee trauma. If the history and physical examination point to damage of the cartilage, the menisci, and the cruciate and collateral ligaments and arthroscopy is contemplated, then magnetic resonance imaging (MRI) is useful for evaluating these structures.
KEY POINTS
- In the emergency department, most patients undergo plain radiography to assess for fracture, yet more than 90% of these studies do not show a fracture.
- CT is useful in patients with knee trauma but normal radiographs.
- MRI is the imaging modality for internal derangement of the knee.
- Ultrasonography’s role in the evaluation of acute knee pain is generally limited to assessment of the extensor mechanism, joint effusion, and popliteal cyst.
PLAIN RADIOGRAPHY STILL THE FIRST STEP IN KNEE EVALUATION
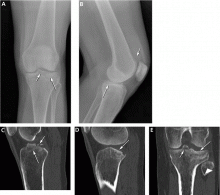
Radiography is the first step in the evaluation of knee pain. It is quick and inexpensive and can yield many diagnostic clues. It can readily reveal fractures, osteochondral defects, bony lesions, joint effusions, joint space narrowing, and bone misalignment.
In patients with knee trauma, supine anteroposterior and cross-table lateral radiographic images are generally obtained. In patients whose knee pain is not due to trauma, standing projections are done, as well as dedicated projection of the patellofemoral articulation. A standing series is most helpful for evaluating joint space and alignment.
Applying the Ottawa rules
When a patient presents to the emergency room with acute knee pain, the immediate concern is whether he or she has a fracture. The Ottawa knee rules9 for when to order radiography in adults with knee pain are highly sensitive for detecting a clinically important fracture. If any one of the five Ottawa criteria applies—ie, the patient is age 55 or older, has tenderness at the head of the fibula, has patellar tenderness, is unable to flex the knee to 90°, or is unable to bear weight—then radiography is indicated.
While studies have validated the ability of the Ottawa rules to detect important fractures in acute knee injury,2,10 fracture is the cause of only a small percentage of knee complaints in the primary care setting. More common causes include osteoarthritis, meniscal injury, ligamental injury, and crystal arthropathy, and these account for approximately half of all diagnoses. Sprain and strain account for most of the rest of knee injuries.1
Acute exacerbations of osteoarthritis
Osteoarthritis is a chronic problem, yet it is not unusual for a patient to present to the primary care physician with an acute exacerbation of joint pain. The clinical hallmarks include age over 50, stiffness lasting less than 30 minutes, bony enlargement and tenderness, and crepitus. The radiographic hallmarks, according to the Kellgren-Lawrence grading scale, are joint space narrowing, osteophytes, subchondral cysts, and sclerosis. These radiographic findings correlate well with clinical findings in these patients.11
Situations in which radiography is less helpful
In some cases the radiographic findings may not explain the patient’s clinical signs and symptoms. For example, in suspected crystalline and septic arthritis, the clinical presentation may include warmth, erythema, and effusion. Arthrocentesis would be indicated in such a patient. Indeed, in the case of suspected pseudogout, chondrocalcinosis may be radiographically evident. However, it is also present in many patients without symptoms or with osteoarthritis, so radiographic evidence does not provide a definite diagnosis.
While radiography may not always identify the cause of knee pain, it is useful in excluding serious problems such as fractures, advanced degenerative changes, and neoplasms, and it may help direct further management. Radiography is not useful in the evaluation of the cruciate and collateral ligaments, the menisci, and the hyaline cartilage of the knee and may fail to show an insufficiency or stress fracture. To evaluate these structures and associated soft tissues, MRI is preferable.
COMPUTED TOMOGRAPHY IN ACUTE KNEE PAIN
CURRENT USES OF MRI TO EVALUATE ACUTE KNEE PAIN
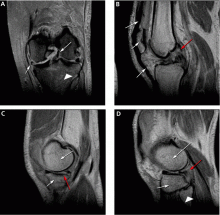
As mentioned above, MRI is useful in evaluating suspected meniscal and ligamentous injuries.
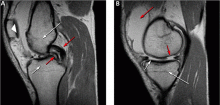
Figure 3 shows how T2-weighted MRI was used to evaluate for suspected meniscal injury in our 47-year-old female patient with left knee pain after a motor vehicle accident.
Still a matter of debate
MRI’s role in the diagnosis of knee pain is still a contentious issue.
Advantages of MRI are that it is noninvasive, it does not use ionizing radiation, it gives multiplanar images, and it provides images of soft-tissue structures, which other imaging methods cannot.12 It is a well-proven and widely accepted test. Its sensitivity for detecting meniscal and cruciate ligament injury ranges from 75% to 88%,1 and it can help in the evaluation of other injuries for which radiography is not useful, including synovitis, bone bruise, stress or insufficiency fracture, osteochondral defects, and osteonecrosis.
In addition, several studies show that using MRI to establish the diagnosis in acute knee pain can mean that 22% to 42% fewer arthroscopic procedures need to be performed.4–8 Authors of a prospective double-blind study8 recommended that MRI be used in patients with acute knee injury when the findings of the clinical history and examination by orthopedic surgeons prove equivocal.8 MRI evaluation is especially desirable for young, active patients who wish to resume activity as soon as possible.
A routine MRI examination consists of T1- and T2-weighted images in three planes, although the number of sequences and planes varies from hospital to hospital. The use of gadolinium contrast is indicated only when osteomyelitis, septic arthritis, or a mass is suspected.
Disadvantages of MRI include its cost: Medicare reimbursement for knee MRI is around $400, compared with $200 for knee CT and $50 for knee radiography with four views. Also, while studies have shown MRI to have a high sensitivity and specificity in the diagnosis of acute knee injury, some have reported a high false-positive rate for the detection of meniscal tear.13,14 MRI has also been shown to have a lower sensitivity than arthroscopy for lesions of the articular cartilage.13 Furthermore, MRI has been shown to reveal cartilage lesions, osteophytes, and meniscal abnormalities in asymptomatic study volunteers with no history of pain, trauma or knee disease.14 Therefore, findings on MRI must closely correlate with findings on the history and physical examination.