An update on proteinuric chronic kidney disease: The dual-goal approach
ABSTRACTLowering both blood pressure and urinary albumin excretion to specific goals may slow the progression of proteinuric chronic kidney disease. However, this dual-goal approach needs to be validated prospectively.
KEY POINTS
- Evidence is emerging that urinary albumin is toxic to the kidney.
- Lowering both blood pressure and urinary albumin excretion, as a means to prevent progressive renal disease, appears to require aggressive inhibition of the renin-angiotensin-aldosterone system, often with several complementary drugs, ie, angiotensin-converting enzyme inhibitors, angiotensin II type 1 receptor blockers, aldosterone receptor antagonists, and possibly, direct renin inhibitors.
- Volume status and potassium levels may help suggest which of several available drugs could be added at different times.
- Serum potassium levels must be managed aggressively when using renin-angiotensin-aldosterone inhibitors in combination.
When angiotensin-converting enzyme (ACE) inhibitors and angiotensin II type 1 receptor blockers (ARBs) were introduced, we hoped that these drugs would slow or stop the inexorable progression of chronic kidney disease. This hasn’t come to pass: the incidence of end-stage renal disease continued to increase throughout the 1990s, and although it may have finally reached a plateau, it remains unacceptably high.1 One reason may be that, used singly, drugs that block the renin-angiotensin-aldosterone system are only moderately successful, as approximately 20% to 40% of patients still reach unfavorable renal end points such as doubling of the serum creatinine level or dialysis.2–7
In view of these disappointing results, some experts are advocating a new strategy in which they advise that both blood pressure and urinary albumin excretion be lowered to specific goals. To achieve these goals, we will generally have to give higher doses of ACE inhibitors and ARBs alone or use a combination of these and other drugs that block the renin-angiotensin-aldosterone system at various sites.
This article describes how the dual-goal approach, with a focus on renin-angiotensin-aldosterone system inhibition, may be applied in the therapy of proteinuric chronic kidney disease. This appears to be a reasonable approach, based on current evidence, to address the epidemic of renal failure. However, further studies are needed to establish the effectiveness of this approach, and the risk of hyperkalemia following aggressive inhibition of the renin-angiotensin-aldosterone system poses a significant management problem.
ALBUMIN MAY BE TOXIC
While hypertension has long been associated with poor renal outcomes, urinary albumin has more recently been implicated by observational and experimental evidence as a tubular-interstitial toxin that may also accelerate the progression of renal disease.
For example, in both the Reduction of Endpoints in NIDDM With the Angiotensin II Antagonist Losartan (RENAAL) study8 and the Ramipril Efficacy in Nephropathy study,4 baseline proteinuria was almost linearly related to worse renal outcomes. In RENAAL, patients who excreted more than about 3 g of albumin per day had an 8.1-fold higher risk of progressing to end-stage renal disease.8 Moreover, the more that protein excretion could be reduced, the better the renal outcomes, down to a level of about 500 mg/day.8
Of importance, lowering blood pressure did not always decrease protein excretion—nearly 40% of patients had a dissociation between the two.9 In fact, prescribing a single ACE inhibitor or ARB while targeting only blood pressure has not predictably reduced protein excretion to 500 mg/day (the proposed goal).2–7
Although albumin has not been conclusively proven to be a renal toxin, targeting the reduction of proteinuria may also succeed if urinary albumin simply serves as a marker of the success of chronic kidney disease treatment and reflects prognosis.
A DUAL-GOAL APPROACH
In view of the observational and experimental evidence, many experts10,15–18 are advocating a dual-goal approach that stresses lowering both blood pressure and urinary protein (albumin) excretion. The recommended goal for systolic blood pressure is less than 120 to 125 mm Hg; the goal for proteinuria is less than 300 to 500 mg/24 hours,16,17,19 aiming to slow the decline in glomerular filtration rate to less than 2 mL/ min/year.11,20
The strategy of targeting both proteinuria and blood pressure has recently received further support. In a prospective randomized controlled study,21 nondiabetic patients with proteinuria received either an ACE inhibitor or an ARB. In one group, the dose was adjusted to lower the blood pressure to less than 130/80 mm/Hg; in the other group, the dose was adjusted to lower the blood pressure to 130/80 and to reduce protein excretion maximally. Only about half as many patients in the group with the dual-goal strategy reached the composite primary end point (doubling of serum creatinine, end-stage renal disease, or death) over a median of 3.7 years of follow-up, as compared with those treated by targeting the blood pressure alone.
In retrospect, the suboptimal success in the earlier landmark studies2–7 may have derived from the failure of ACE inhibitors and ARBs, used by themselves at moderate doses, to either lower the blood pressure to the recently advised goal (the actual results obtained varied from about 128 to about 145 mm Hg systolic) or, perhaps, to reduce proteinuria to the goal level.
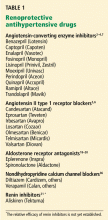
Not all nephrologists currently pursue the stringent proteinuria goal of 500 mg per day—the targeted reduction of proteinuria requires further prospective evidence to support it. However, nephrologists do commonly follow the broad theme that antihypertensive therapy in proteinuric chronic kidney disease should accentuate medicines that protect the kidney beyond their antihypertensive effect (Table 1), and that proteinuria is an important metric that, at the very least, reflects the response to therapy and prognosis.