Thoracic aortic aneurysm: How to counsel, when to refer
ABSTRACT
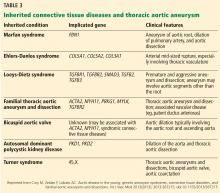
Thoracic aortic aneurysm (TAA) is usually clinically silent and progresses slowly until a tipping point is reached, after which the aortic diameter can expand more rapidly and the condition can potentially end in aortic dissection or rupture. Causes include bicuspid aortic valve and genetic syndromes (Marfan, Loeys-Dietz, and Ehlers-Danlos syndromes) and familial associations, but many cases are idiopathic. Clinicians should therefore be alert for clues on chest imaging, and consider screening in first-degree relatives of patients known to have aortic disease. Early referral to a cardiologist specializing in aortic disease is key.
KEY POINTS
- Screening and referral depend on clinical context. A size-based model to determine screening, referral, follow-up, and management serves most cases but should be modified in the context of connective tissue disease or family history of aneurysm and dissection.
- Medical management involves strict blood pressure and heart rate control with beta-blockers and angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers. Activity modifications should be tailored to the individual, although extreme isometric exercises and heavy lifting should be discouraged.
- Patients with TAA should be followed up annually, unless the patient is presenting for initial evaluation or significant changes are seen with dedicated imaging.
HOW IS TAA DIAGNOSED?
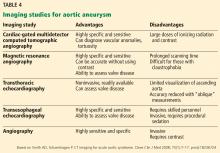
Imaging tests
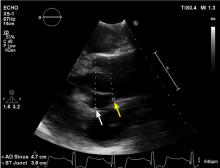
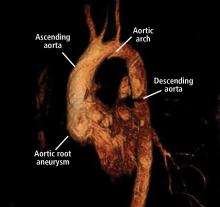
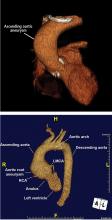
It is particularly important to obtain a gated CTA image in patients with aortic root aneurysm to avoid motion artifact and possible erroneous measurements. Gated CTA is done with electrocardiographic synchronization and allows for image processing to correct for cardiac motion.