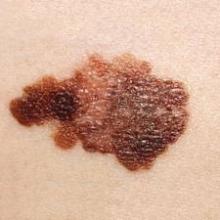
Melanoma increases in adolescents
FROM PEDIATRICS
Since the 1970s, the incidence of melanoma has been rising about 2% per year in adolescents, the same as it has in adults, according to an epidemiologic study published online April 16 in Pediatrics.
The reasons for this increase are not yet clear. Individual-level studies rather than population-level studies are needed to find the explanation for this trend, said Jeannette R. Wong of the division of cancer epidemiology and genetics at the National Cancer Institute, Rockville, Md., and her associates.
Recent studies have documented the increase in adult melanoma cases and "illuminated likely contributing factors," but none have assessed childhood and adolescent melanoma, the researchers noted. They analyzed data from the Surveillance, Epidemiology, and End Results (SEER) database for nine U.S. geographic regions from 1973 through 2009. They identified all first melanomas diagnosed among patients aged 19 years and younger.
A total of 1,317 cases of melanoma were identified during the study period. Because few of the malignancies developed in nonwhite patients or in patients of unknown race/ethnicity, only the 1,230 cases that developed in white patients were included in the analysis.
The overall incidence of melanoma rose by an average of 2% per year for both boys and girls (Pediatrics 2013 April 16 [doi: 10.1542/peds.2012-2520]).
Melanoma was nearly twice as common in girls compared to boys overall (61% vs. 39%) with similar percentages within each age group (0-9 years, 10-14 years, and 15-19 years).
The incidence increased with age. The majority of melanomas – 77% – were diagnosed in adolescents aged 15-19 years. Only 8% of melanomas were diagnosed in children aged 9 years and younger, and 15% were diagnosed in those aged 10-14 years.
The incidence of localized melanoma was much higher (77%) than that of regional (13%), distant (2%), or unstaged disease (8%).
The most frequent melanoma sites in girls were the lower limbs and hips, on which melanomas increased by a significant annual percentage change of 3% over the study period. Among boys, melanomas were most common on the skin of the face and trunk, with annual percentage increase of 5% over the study period.
UVB exposure did not appear to be the primary factor contributing to the increase in melanoma, the researchers noted. In fact, melanoma rates were slightly higher in geographic areas that had low UVB exposure (such as Connecticut and Washington state) than in areas with high UVB exposure (such as Hawaii and California). "However, all significantly increasing trends for melanoma over our study period occurred in sun-exposed areas of the body," they said.
This finding suggests that tanning facilities may instead be a major source of the increase in incidence, because there are many more such facilities in low-UV regions, the researchers said.
Increased use of tanning facilities also may explain why the rate of melanoma is higher in girls than in boys, since girls are much more likely than boys to use such facilities, they added.
It is also possible that heightened awareness of melanoma in recent years has improved detection rates in the pediatric population, the researchers said.
These data are consistent with those of previous studies that have reported increasing rates of melanoma in the pediatric populations of Australia, Sweden, and England.
Although this study included more than 30 years of data on melanoma incidence, it was limited in that it did not include individual-level data on outdoor UV exposure, use of tanning facilities, or familial factors related to melanoma risk, the researchers said.