Bilateral axillary rash
A 53-year-old woman went to a new family physician (FP) because she was concerned about a bilateral axillary rash that she’d had for the past year. The patient said the area under her arms was itchy and occasionally painful. She’d stopped using deodorant because it would sting. The FP noted small pits in 2 of her fingernails. Her previous doctor had prescribed a number of topical and oral antifungal medications over the previous year, but they hadn’t helped.
What’s your diagnosis?
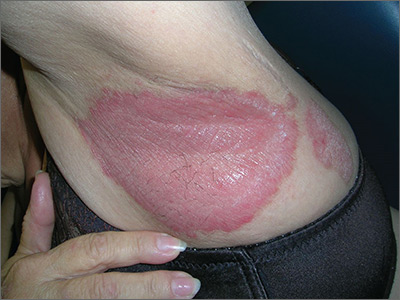
The FP diagnosed inverse psoriasis. Important clues that pointed to the diagnosis included the history of the rash not resolving with antifungal medications or after stopping use of deodorant (evidence that this was unlikely to be contact dermatitis), along with the fingernail pits.
Inverse psoriasis is found in the intertriginous areas of the axillae, groin, inframammary folds, and intergluteal fold. “Inverse” refers to the fact that the distribution is not on extensor surfaces, but in areas of body folds. Morphologically, the lesions have little to no visible scale and, therefore, are not easily recognized as psoriasis. The color is generally pink to red, but can be hyperpigmented in dark-skinned individuals.
Inverse psoriasis often mimics Candida and tinea infections; when antifungal medicines are not working, always consider inverse psoriasis. Not all erythematous plaques in the axillae are fungal. It helps to look for clues such as nail changes (such as the pits noted with this patient) or subtle plaques on the elbows, knees, or umbilicus to make the diagnosis of psoriasis.
Treatment consists of a mid- to high-potency topical steroid. The choice of vehicle can be based on patient preference; creams and ointments both work to treat inverse psoriasis.
In this case, the FP prescribed a mid-potency topical corticosteroid (0.1% triamcinolone ointment) to be applied twice daily. Both the FP and the patient agreed that an ointment, rather than a cream, would be the better option. While the ointment can be greasy, creams often have an alcohol base and are thus more likely than a petrolatum ointment to sting.
The FP also checked for psoriasis risk factors and discovered that the patient was neither smoking nor drinking alcohol. However, the patient was overweight and agreed to improve her diet and exercise for reasonable weight loss.
At her follow-up 2 months later, the patient’s psoriasis was 90% better. She had also lost 5 pounds. While discussing treatment options, a joint decision was made to try a higher-potency topical steroid ointment with the goal of 100% clearance. The patient understood the risk of skin atrophy and was given instructions to return to the mid-potency steroid once the higher-potency steroid achieved satisfactory results.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Usatine R. Psoriasis. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013: 878-895.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com




