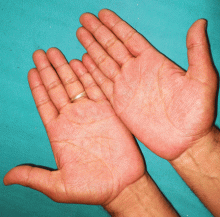
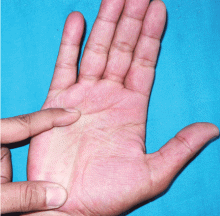
Painful red hands and feet
Q: What is the diagnosis?
- Fabry disease
- Peripheral neuropathy
- Polycythemia
- Primary idiopathic erythromelalgia
- Erythrodysesthesia syndrome
A: The correct diagnosis is primary idiopathic erythromelalgia.
Erythromelalgia is a relatively rare clinical condition of uncertain etiology, characterized by the triad of episodic redness, warmth, and burning pain in the extremities.1,2
,The condition has primary (ie, no underlying cause is found) and secondary forms.1,3 The primary form may be inherited in an autosomal dominant manner (in which case the symptoms begin in childhood), or it may be idiopathic.4 On the other hand, erythromelalgia can also be secondary to polycythemia vera and other myeloproliferative disorders, connective tissue disorders, neuropathies, spinal cord diseases, carcinoma of the colon and thyroid, and astrocytomas.1–6
The common pathologic mechanism of erythromelalgia is thought to be microvascular arteriovenous shunting.5 A mutation in the voltage-gated sodium channel alpha subunit NaV1.7 may result in primary erythromelalgia. Small-fiber neuropathy2 can manifest as erythromelalgia and may respond to steroids.
The symptoms can be intermittent or, in rare cases, constant.3 The lower limbs are more commonly involved than the upper ones.3 Involvement is often bilateral and symmetric.3 The symptoms may worsen at night, after alcohol consumption, with higher environmental temperature, and with moderate exercise.3 In rare cases, ulceration and gangrene may occur. Patients may get relief by cooling the affected areas.2
DIAGNOSIS BY EXCLUSION OR BASED ON THE PRESENTATION
The diagnosis of erythromelalgia is based on a detailed history and physical examination during a painful episode.2,3 Because the condition is intermittent, only about two-thirds of patients have abnormal findings on physical examination at the time of presentation; in such cases, the diagnosis is based on the history alone.2
Testing is needed to exclude other diagnoses and to determine the cause of secondary erythromelalgia. Histopathologic study of lesions is not helpful, as the features are nonspecific and hence nondiagnostic.2
In our patient, the typical clinical features and the lack of an obvious cause on diagnostic testing confirmed the diagnosis.
THE DIFFERENTIAL DIAGNOSIS
Other conditions can be ruled out by clinical features and laboratory testing.
Fabry disease causes paresthesia and burning pain in the extremities but not erythema. Characteristic dark red keratotic papules are seen all over the body (angiokeratoma corporis diffusum). It is often associated with progressive renal insufficiency.
Peripheral neuropathy of varying causes may also cause pain in the extremities but not erythema. Neurologic examination and a nerve conduction velocity study can resolve the diagnostic problem. Clinical features and laboratory testing often help to pinpoint the cause of neuropathy.
Polycythemia may cause erythema in the hands, feet, and face and mucosal engorgement. Telangiectasia, petechiae, and cyanosis may also occur. Our patient’s normal complete blood cell count excluded this condition.
Erythrodysesthesia syndrome, typically caused by chemotherapeutic drugs, was not included in the differential diagnosis since our patient had taken no medications.
Other causes of palmar erythema to rule out, depending on the patient’s presentation, may include thyrotoxicosis, chronic febrile illness, leukemia, hepatic insufficiency, chronic alcoholism, and rheumatoid arthritis.
TREATMENT AND PROGNOSIS
There is no definitive therapy for erythromelalgia.4 Treatment is often difficult and needs a multidisciplinary approach. Simple measures such as cooling2 (eg, applying cold towels, immersion in cool water, walking on cold floors) or elevating the affected extremity often relieve symptoms. Patients should avoid precipitating factors such as warmth, dependency of extremities, exercise, tight footwear, and alcohol intake.
If there is an underlying disease, treating the disease may also alleviate the symptoms.7 Aspirin2,7 is the therapy of choice for erythromelalgia in patients with an underlying myeloproliferative disorder, and some authors have advocated it for all patients with erythromelalgia unless there is a contraindication.7
Other possible first-line treatments include the synthetic prostaglandin E1 analogue misoprostol (Cytotec) and prostacyclins. Gabapentin (Neurontin), serotonin reuptake inhibitors such as sertaline (Zoloft) and venlafaxine (Effexor), and intravenous nitroprusside (Nitro-press) are considered second-line drugs.7
Surgical sympathectomy8 has also been tried, with variable results.
Outcomes in patients with erythromelalgia
In a case series from Mayo Clinic,2 approximately equal numbers of patients with erythromelalgia became worse, stayed the same, or got better, and the disease resolved in 10% over a mean of 8.7 years.
THE OUTCOME IN OUR PATIENT
We advised our patient to avoid strenuous activity in a warm environment and to work in cooler areas as much as possible. We told him to wrap his affected extremities with cold towels during attacks, and we prescribed aspirin (650 mg/day) for 3 months. The treatment did not cure his condition, but his symptoms lessened within 2 months. We later referred him to a pain clinic.