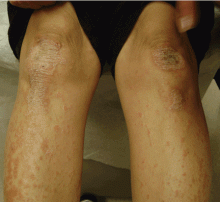
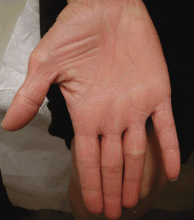
A rash on the legs and palms
Q: Which is the most likely diagnosis?
- Psoriasis
- Pityriasis rubra pilaris
- Dyshidrotic eczema
- Keratoderma
- Contact dermatitis
A: The diagnosis is pityriasis rubra pilaris, a rare condition with a prevalence of 1 in 5,000 to 50,000 new dermatology patient visits.1 It is a papulosquamous disorder that presents with areas of hyperkeratosis on an erythematous base. Large red plaques often coalesce, leaving areas of uninvolved skin (“islands of sparing”). The palms and soles often reveal a distinctive orange-red waxy keratoderma.1
Clinically, pityriasis rubra pilaris can be difficult to differentiate from psoriasis, and it can progress to disabling palmoplantar keratoderma and erythroderma.
,BASIS OF THE DIAGNOSIS
The diagnosis is based on characteristic findings supported by classic features on skin biopsy. Microscopic study shows a psoriasiform dermatitis with alternating vertical and horizontal orthokeratosis and parakeratosis (the “checkerboard pattern”).
Although an underlying dysfunction in vitamin A metabolism has been suggested, the exact cause and pathogenesis of pityriasis rubra pilaris are not known.
TREATMENT
Treatment of pityriasis rubra pilaris can be difficult, as no one single treatment works for all patients. Systemic retinoids, methotrexate, phototherapy, and cyclosporine are commonly used. Recent reports have shown the effectiveness of infliximab (Remicade), a chimeric monoclonal antibody that binds to soluble and membrane-bound forms of tumor necrosis factor alpha.2,3
In our patient, after a 2-month course of acitretin (Soriatane) failed, three treatments with infliximab—5 mg/kg at baseline, at 2 weeks, and at 6 weeks—led to complete resolution of the condition.