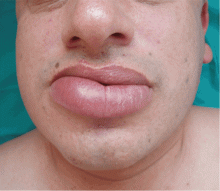
A persistently swollen lip
A 44-year-old man is referred for evaluation of asymptomatic swelling of the lower lip that has persisted for 10 months. He has been treated unsuccessfully with oral antihistamines for suspected chronic angioedema. He has no other symptoms and appears to be well otherwise. He has no history of applied irritants or local trauma, and his medical history is unremarkable.
Results of the laboratory evaluation, including serum angiotensin-converting enzyme level, are normal. Patch tests to detect contact sensitivity to food additives are negative. Biopsy of the affected lip reveals dense infiltrate of the submucosal connective tissue with focal nonnecrotizing granulomas. Imaging and endoscopic studies show no evidence of sarcoidosis or Crohn disease.
Q: Given what we know so far, which of the following is the most likely diagnosis of the persistent lip swelling?
,- Melkersson-Rosenthal syndrome
- Amyloidosis
- Quincke edema
- Cheilitis granulomatosa
- Cutaneous tuberculosis
A: From what we know so far, the correct answer is cheilitis granulomatosa. While this rare condition may be a feature of Melkersson-Rosenthal syndrome and amyloidosis, at this point in the evaluation these have not been confirmed. Quincke edema (ie, angioedema) is unlikely, given the ineffectiveness of previous treatment with oral antihistamines. Cutaneous tuberculosis usually presents as “lupus vulgaris,” which is characterized by solitary, small, sharply marginated, red-brown papules of gelatinous consistency (“apple-jelly nodules”), mainly on the head and neck.
Cheilitis granulomatosa is a rare inflammatory disorder1 that primarily affects young adults. Its key feature is recurrent or persistent painless swelling of one or both lips. It may occur without other signs of disease, but it is also a manifestation of Melkersson-Rosenthal syndrome and it may be a presenting symptom of Crohn disease or, rarely, sarcoidosis.2 The term “orofacial granulomatosis” was introduced to encompass the broad spectrum of nonnecrotizing granulomatous inflammation in the orofacial region, including cheilitis granulomatosa, the complete Melkersson-Rosenthal syndrome, sarcoidosis, Crohn disease, and infectious disorders such as tuberculosis.1
The cause of cheilitis granulomatosa is unknown. Specific T-cell clonality has been identified in several patients with orofacial granulomatosis, suggesting a delayed hypersensitivity response. Moreover, the HLA haplotypes HLA-A2 and HLA-A11 have been found in 25% of patients with orofacial granulomatosis, suggesting a viral etiology. A genetic predisposition may exist in Melkersson- Rosenthal syndrome: siblings have been affected, and otherwise unaffected relatives may have a fissured tongue (lingua plicata).
Melkersson-Rosenthal syndrome, a rare condition, is characterized by a classic triad of recurrent swelling of the lips or face (or both), fissured tongue, and relapsing peripheral facial nerve paralysis. It is an unusual cause of facial swelling that can be confused with angioedema.3 This syndrome can be ruled out in this patient because he has only one of the three classic signs. Contact antigens are sometimes implicated.
DIFFERENTIAL DIAGNOSIS OF CHEILITIS GRANULOMATOSA
The differential diagnosis of cheilitis granulomatosa is extensive and includes amyloidosis, cheilitis glandularis, sarcoidosis, Crohn disease, actinic cheilitis, neoplasms, and infections, such as tuberculosis, syphilis, and leprosy.1
As many as 11% of patients with Crohn disease may develop mucocutaneous lesions. Oral lesions of Crohn disease include apthae, cobblestoning of the buccal mucosa, swelling of one or both lips (soft or rubbery), vertical clefts of the lips, or hypertrophic gingivitis. Only 5% of patients with Crohn disease ever develop cheilitis granulomatosa, though most cases occur in children.
Ultimately, the diagnosis of cheilitis granulomatosa is made by correlating the patient’s history and clinical features, usually supported by histopathologic findings of nonnecrotic granulomas extending into the deep dermis, composed of histiocytes and giant cells and associated with a lymphomonocytic infiltrate.
TREATMENT
Treatment of cheilitis granulomatosa is difficult because the cause is unknown and the rate of recurrence is high. Response to treatment is often late and unpredictable. Corticosteroids, clofazimine (Lamprene), and surgical intervention such as cheiloplasty have been described as treatment options. Other treatment options include thalidomide (Thalomid), sulfasalazine (Sulfazine), erythromycin, azathioprine (Imuran), and cyclosporine (Sandimmune). Infliximab (Remicade) has been recently reported as a new alternative treatment, in particular for Melkersson-Rosenthal syndrome.4
In our patient, twice-monthly injections of 1 mL of triamcinolone acetonide 10 mg/mL into the affected lip brought acceptable improvement at 3 months. The patient is on maintenance treatment with twice-monthly triamcinolone injections and has had no relapses after 2 years.