Dermatology for the pediatrician: Advances in diagnosis and treatment of common and not-so-common skin conditions
ABSTRACTAdvances have been made in understanding and treating both common and rare dermatologic conditions. Atopic dermatitis benefits from bathing and ceramide moisturizers. Common allergic contact dermatitis may have specific presentations. Tinea capitis is effectively treated with terbinafine. Infantile hemangiomas should be treated early in the disease course and respond well to propranolol; any white sign of ulceration should be noted. Localized alopecia areata responds well to topical clobetasol, avoiding the need for intralesional injections. Topical rapamycin can be used to treat tuberous sclerosis. Further understanding of genetics will help guide pediatricians to the proper diagnosis and treatment of skin conditions.
Primary care pediatricians are often asked about manifestations of both common and rare dermatologic disorders. They frequently encounter pediatric skin conditions, making it important to stay abreast of new developments in diagnosis and treatment. Common pediatric dermatologic diagnoses include atopic dermatitis, allergic contact dermatitis, tinea capitis, infantile hemangioma, and alopecia areata. Less common conditions include epidermal nevi and tuberous sclerosis.
ATOPIC DERMATITIS (ECZEMA)
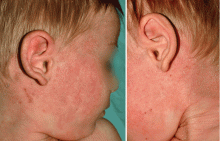
Atopic dermatitis, also referred to as eczema, is a common pediatric skin condition characterized by erythema, pruritus, scaling, lichenification, and papulovesicles (Figure 1). It affects up to 17% of children in the United States.1,2 A wide range of environmental factors, such as contact allergens, stress, food, skin flora, and humidity, affect the development and severity of atopic dermatitis. Studies also support a genetic basis; when both parents are atopic, their children have a 70% risk for developing atopic dermatitis.3
Approximately 50% of European whites have a filaggrin mutation thought to cause pediatric atopic dermatitis or eczema. The filaggrin gene (chromosome 1q21) is located in the epidermal differentiation complex and encodes profilaggrin. The defect leads to a poor protein-lipid cell envelope and a loss of the filaggrin hygroscopic amino acids that act as a natural barrier.4
Additionally, these patients have increased surface pH. This is of particular importance because at a certain pH, there is decreased inhibition of Staphylococcus aureus. Decreased activity of ceramide metabolism enzymes occurs, resulting in increased water loss along with increased entry of foreign substances.
The best treatment for atopic dermatitis is daily bathing with a mild, nondrying soap. Unfortunately, many parents purposely do not bathe their atopic children daily because they believe it is harmful. Many mild cleansers are available today that do not aggravate the condition.
Another effective treatment for eczema is to apply a moisturizer. Previously, thick ointments likely to occlude water loss were applied, but research on the pathophysiological process of atopic dermatitis has led to the development of moisturizers and topical skin products targeted to correct reduced amounts of ceramides and natural moisturizing factors in the skin with natural moisturizing factors, ceramides, and pseudoceramide products.5 A ceramide-containing moisturizer should be applied immediately after giving the child a bath. These moisturizers are available over-the-counter but can be relatively expensive. Some popular ceramide-containing skin lubricants include CeraVe cream, Cetaphil RestoraDerm cream, Aveeno eczema cream, and Eucerin eczema cream. If cost is an issue, a thick emollient such as petroleum jelly can be used.
Prevention
Several theories have been proposed to explain the development of eczema beyond genetic predisposition, leading to attempts to prevent its development. Theories include breastfeeding—both nursing and not nursing. While it seems that breastfeeding should be protective against atopic dermatitis, unfortunately there is no proof of this. Also, withholding certain foods during the introduction of solid foods (and not eating certain foods during nursing) will not decrease the risk of developing atopic dermatitis. Early exposure to farm animals has been debated as causative, and there is evidence that early exposure to antibiotics increases atopic dermatitis risk. Lastly, maternal fish oil or probiotic ingestion during pregnancy has not changed the rates of atopic dermatitis in infants.6,7 Therefore, the best course of action is to provide simple skin care guidelines and treat children as they present with atopic dermatitis.
ALLERGIC CONTACT DERMATITIS
Contrary to previously held beliefs, allergic contact dermatitis is not rare in children. In fact, rates are equal between children and adults. Allergic contact dermatitis or irritant contact dermatitis is also associated with skin barrier breakdown common among atopic dermatitis patients. Additionally, atopic dermatitis patients may exhibit allergic contact dermatitis due to exposure to various topical preparations.8
Toilet seats
Recently, allergic contact dermatitis has been reported in association with toilet seats,9 possibly due to polyurethane or polypropylene in the seat.10 Another possible reaction may be to chemicals in antiseptic wipes used on the toilet seat. The presentation of allergic contact dermatitis due to toilet seat contact is higher on the posterior thigh for older children compared to that seen in toddlers and younger children. It can be differentially diagnosed from atopic dermatitis because it is limited to the posterior leg.11
Baby wipes
Some baby-wipe brands contain the allergen methylisothiazolinone, alone or in combination with methylchloroisothiazolinone.12 Even expensive brands marketed as hypoallergenic may contain these chemicals or other types of preservatives. Interestingly, some parents continue to use baby wipes on their children’s faces and bodies as they grow up to provide a quick clean up. So, in children who are toddler age or older, allergic contact dermatitis to baby wipes may not be localized to the anogenital area. Consider this condition in the differential diagnoses with “lip licker” dermatitis.