Sleep apnea ABCs
To the Editor: We read with interest the paper by Dr. Reena Mehra,“Sleep apnea ABCs: Airway, breathing, circulation.”1 It was very consistent and informative. However, we feel that some considerations on the pathogenesis warrant more discussion.
The pathophysiologic heterogeneity of sympathetic nervous system activity enhancement is complex and involves both intermittent hypoxia and arousal. We agree with Dr. Mehra about the importance of intermittent hypoxia in sympathetic activation, and we would like to point out the importance of effects of arousal from sleep on autonomic outflow. In some patients with obstructive sleep apnea (OSA) in whom respiratory events are not followed by oxygen desaturation, sympathetic activation cannot be explained by intermittent hypoxia. Arousal has been reported to be associated with an acute increase in sympathetic activity in the absence of hypercapnia or hypoxia.2 Cortical arousals from sleep have been historically assumed to be important in restoring airflow at the end of OSA breathing events.3 Furthermore, arousals often precede upper-airway opening in patients with OSA.4
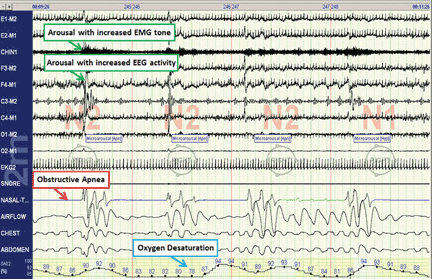
In Figure 1 of Dr. Mehra’s paper, all the respiratory events were associated with microarousals. According to the conventional definition, cortical arousal is an abrupt shift in the electroencephalogram lasting more than 3 seconds. In Figure 1, the beginning of arousals must be scored a few seconds before breathing recovery, just at the beginning of electroencephalogram acceleration. The second respiratory event was scored as obstructive apnea, or the apnea started out as central apnea, where all respiratory channels are flat and then the chest and abdominal belts start moving, making it look like typical mixed apnea.
,In the title of the paper, the “A” of ABCs referred to airway and, more specifically, to the collapse of the upper airway in sleep, which is the cause of OSA. We think that the “A” can be attributed to arousal, which is specific to sleep and contributes to the pathogenesis of OSA.




