Interventionalists skeptical about public reporting of PCI
FROM JAMA CARDIOLOGY
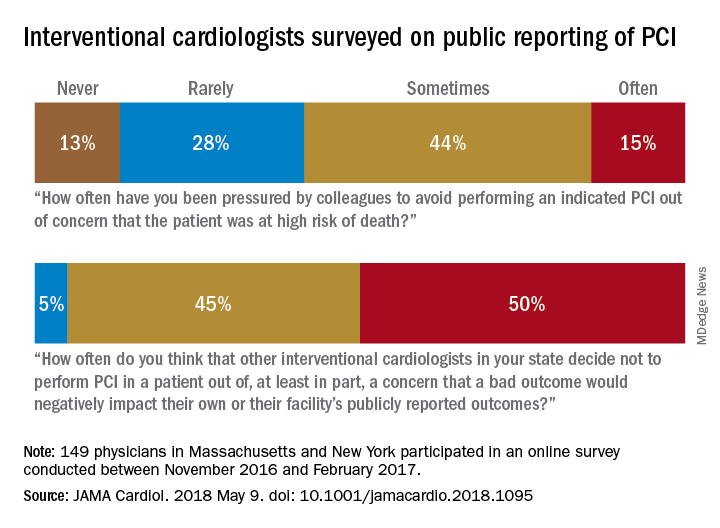
Many interventional cardiologists believe that public reporting of percutaneous coronary intervention (PCI) outcomes leads to avoidance of high-risk procedures and “purposeful upcoding of comorbidities by colleagues,” according to a survey of 149 interventionalists.
Almost 60% of respondents said that they were sometimes or often pressured by other physicians to not perform PCI on patients considered to be at high risk of death, and 95% believed that other interventionalists in their state – the survey was conducted in New York and Massachusetts – would sometimes or often avoid PCI because of “concern that a bad outcome would negatively impact their own or their facility’s publicly reported outcomes,” Daniel M. Blumenthal, MD, MBA, of Massachusetts General Hospital, Boston, and his associates said in an article published online May 9 in JAMA Cardiology.
Almost two-thirds of participants said that they had avoided performing PCIs at least twice because they were worried about reporting a negative outcome, which “suggests that PCI avoidance is not concentrated among a few risk-averse interventionalists,” Dr. Blumenthal and his associates wrote.
Their study was supported by an unrestricted research grant from Abiomed to the Smith Center for Outcomes Research in Cardiology at Beth Israel Deaconess Medical Center. Dr. Blumenthal reported consulting fees and/or funding for unrelated work from Devoted Health, Novartis Pharmaceuticals, HLM Venture Partners, and Precision Health Economics.
SOURCE: Blumenthal DM et al. JAMA Cardiol. 2018 May 9. doi: 10.1001/jamacardio.2018.1095.




