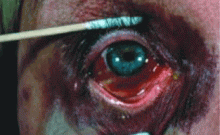
Red eye for the internist: When to treat, when to refer
ABSTRACTWhen a patient presents with redness in the eye, the cause needs to be diagnosed quickly. Some of the diseases that cause redness in the eye can be initially managed by an internist, but others call for quick referral to an ophthalmologist. This article reviews the spectrum of conditions manifesting as a red eye, emphasizing how to differentiate between the benign and the vision-threatening.
KEY POINTS
- Blepharitis, conjunctivitis, corneal abrasion, dry eye, and subconjunctival hemorrhage are benign and can usually be managed initially by an internist, although referral is usually indicated if symptoms persist or progress.
- Patients with corneal bacterial infection, uveitis, scleritis, or acute narrow-angle glaucoma need immediate referral to an ophthalmologist, as do most patients with a red eye who use contact lenses, who have had trauma to the eye, or who have vision changes, severe pain, nausea, vomiting, severe headache, marked purulent discharge, or abnormalities in the cornea or anterior segment.
- Because it is difficult to distinguish between infectious and noninfectious conditions, and because treating infections with corticosteroids alone can have grave consequences, we recommend that internists generally not use topical corticosteroids to treat eye symptoms.
Many patients present to internists because of redness in the eye. The possible causes range from benign (which generally can be handled by an internist) to vision-threatening (which need prompt or emergency referral to an ophthalmologist).
HISTORY HELPS IDENTIFY THE CAUSE
The internist should ascertain:
- Whether one or both eyes are affected
- The duration of symptoms
- Previous eye and medical problems
- The type of discharge (watery or purulent), if present
- Whether the patient has any visual changes, pain, or photosensitivity.
Refer patients to an ophthalmologist for further evaluation if they use contact lenses or if they have had trauma to the eye, vision changes, severe pain, or systemic symptoms such as nausea, vomiting, or severe headache.
BASIC EYE EXAMINATION
Examine:
- Visual acuity
- Pupil size and reaction to light
- The pattern and location of the redness
- The cornea and anterior segment for gross abnormalities such as corneal opacities, hypopyon (a layer of inflammatory cells in the anterior chamber), and hyphema (hemorrhage in the anterior chamber) (Use a penlight.)
- The preauricular lymph nodes. Preauricular lymphadenopathy, detected by palpation, suggests but is not specific for viral conjunctivitis.
- Funduscopy has little value in evaluating a red eye.
Refer immediately anyone who has marked purulent discharge or abnormalities in the cornea or anterior segment.
CONDITIONS A GENERALIST CAN INITIALLY MANAGE
Subconjunctival hemorrhage
Subconjunctival hemorrhages are harmless and do not cause pain or vision changes. No treatment is required, and the blood resorbs within a few weeks. However:
- Measure the blood pressure—uncontrolled hypertension can present with subconjunctival hemorrhage.1
- If the patient is on an antithrombotic agent, test the prothrombin and activated partial thromboplastin times.
- If the patient has recurrent unexplained episodes of subconjunctival hemorrhage, look for a bleeding disorder such as von Willebrand disease, hemophilia, or autoimmune thrombocytopenic purpura.
Blepharitis
Blepharitis, a common condition, is inflammation of the eyelid margins. Anterior blepharitis affects the eyelashes and anterior eyelid margin and is most often caused by a low-grade staphylococcal infection or seborrheic dermatitis. Posterior blepharitis involves the orifices of the slender sebaceous glands of the eyelids (the meibomian glands) and is often associated with acne rosacea.
Symptoms include ocular burning, a sensation that a foreign body is in the eye, and watering. Symptoms are typically worse in the morning and gradually improve throughout the day. Although the onset is sudden in some patients, blepharitis is usually chronic—often lifelong—and starts insidiously.
A sign of anterior blepharitis is crusting around the eyelashes. Patients with concomitant seborrheic dermatitis also have oily skin and flaking from the eyebrows and scalp. Signs of posterior blepharitis are oil inspissation around the meibomian gland openings, telangiectasias of the eyelid margin, and accompanying acne rosacea (skin pustules, telangiectasias, and erythema).
Treat both forms with eyelid hygiene: applying warm compresses to the eyelid margins, followed by gentle massage to remove the debris from the eyelashes and meibomian glands. This is done two to four times daily until acute symptoms resolve, then once daily. Because blepharitis is chronic, eyelid hygiene must be continued indefinitely to prevent acute exacerbations.
Posterior blepharitis that does not respond to hygiene can be also treated with oral tetracycline, which is believed to improve meibomian gland function and alter bacterial colonization.
Some patients also have tear deficiency, which can be addressed with tear replacement therapy (see below).2,3